Acute Pancreatitis
"The prognosis of acute pancreatitis is very variable, since the evolution can go from very benign and without complications to catastrophic and fatal".
DR. CÉSAR PRIETO
SPECIALIST. DIGESTIVE DEPARTMENT

Acute pancreatitis consists of an acute inflammation, of sudden onset, of more or less intensity, in which, after the episode, the form and function of the gland is completely recovered.
The main mechanism that triggers the inflammation is, for some reason, the alteration in the control mechanisms of enzyme secretion, producing a secretion "inwards" from the gland itself instead of towards the duodenum, originating a true autodigestion of the pancreas and sometimes of neighboring organs.

What are the symptoms of acute pancreatitis?
The primary symptom that is present in over 95% of acute pancreatitis cases is abdominal pain.
It is usually a poorly tolerated pain, of moderate or severe intensity, located in the upper or middle part of the abdomen, in a bar arrangement, which is transmitted like a dagger to the back, and which invites the patient to maintain quietness and curl up. This pain usually has a precise beginning and is reported by the patient or his or her family.
Other very frequent symptoms, present in up to 80 or 90% of cases, are nausea and vomiting, initially food and later watery or bilious. Two other common symptoms, although somewhat less frequent, are fever and abdominal distension.
Most common symptoms:
- Abdominal pain.
- Nausea and vomiting.
- Fever.
- Abdominal distension.
In mild pancreatitis, of more benign course, the most frequent symptom is moderate pain with or without nausea or vomiting.
These symptoms have an abrupt and progressive beginning and last from hours to weeks or months, depending on the severity, the course the disease takes and the means put in place to treat it.
Do you have any of these symptoms?
You may have acute pancreatitis
What are the causes of acute pancreatitis?
The causes of acute pancreatitis are multiple, but overall more than 80% can be attributed to three main causes:
More than half of the cases are due to stones coming out through the bile duct, which ends, together with the pancreas, in the duodenal papilla. These stones usually come from the gallbladder or the bile duct.
In about a quarter of the cases, it is the excessive consumption of alcohol.
Pancreatitis of non-filiate origin, includes those cases for which none of the known causes were demonstrated.
Other causes, which together represent less than 10%, are having excessive levels of fat in the blood (hyperlipemia), endoscopic explorations of the biliary and pancreatic duct, postoperative of major surgeries, structural alterations of the pancreatic and duodenal region either congenital or acquired, alterations in the function of the parathyroid gland, abdominal trauma, drugs, infections and other much rarer.
Who can suffer from it?
In Spain, the incidence of acute pancreatitis ranges from 100 to 400 new cases per year per 100,000 inhabitants.
Any previously healthy person can suffer from acute pancreatitis, but the rule is that it occurs in people who suffer from one of the predisposing causes. Having stones in the gallbladder or possessing stone-forming bile is a risk factor. Two out of every three patients with pancreatitis caused by stones are women. The greatest frequency occurs between the ages of 50 and 70.
Another cause is alcohol consumption, which can produce acute pancreatitis depending on the amount ingested, the chronicity of the intake, nutritional habits and other predisposing factors of the patient. Three out of every four patients with acute alcohol pancreatitis are male. The age of presentation is between 30 and 50 years old.
How is acute pancreatitis diagnosed?
The diagnosis of acute pancreatitis has three basic pillars:
- The most important one is that the symptoms coincide with those described, so the doctor's experience is fundamental to guide towards an accurate diagnosis.
- The second pillar is the increase in the blood of some enzymes secreted by the pancreas, such as amylase and lipase.
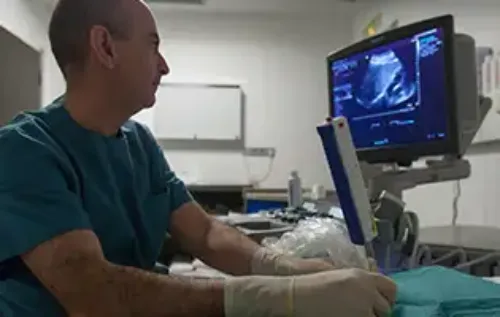
- The last pillar is to demonstrate by some imaging technique (ultrasound or scanner) that there are changes in the shape and/or size of the pancreas or alterations in its vicinity.
How is acute pancreatitis treated?
Treatment of acute pancreatitis should always be on an inpatient basis, even in an intensive care unit for the first few hours or longer if necessary.
The treatment should be adjusted to each case, trying to anticipate the events that may appear in the evolution.
The basic points are: a close control of the patient (vital signs and multiple and serial analytical tests); the treatment of pain with powerful analgesics, including opiates; maintaining an adequate hydration and nutrition of the patient through the vein, avoiding food by mouth; specific treatment of nausea and vomiting; blocking the gastric secretion of acid with drugs, antibiotics by vein to avoid infections that would shadow the evolution.
In cases of acute pancreatitis due to stones in the bile duct, it is indicated to try to extract the stone through endoscopic procedures.
What clinical trials do we have on Acute Pancreatitis?
The Department of Digestive
of the Clínica Universidad de Navarra
The Digestive Department of the Clinica Universidad de Navarra is composed of a multidisciplinary team of specialists who are experts in the diagnosis and treatment of diseases of the digestive tract.
Our objective is that each diagnosis be carefully established and the treatment plan adjusted to each patient.

Why at the Clinica?
- Medical specialists who are national references.
- Specialized nursing team.
- Endoscopy Unit and High Risk Digestive Tumor Prevention and Consultation Unit to offer the best care to our patients.















