Diverticulosis and diverticulitis
"Between 5-10% of the general population has colon diverticula, being much more frequent in people over 50, increasing their number with age".
DR. RAMÓN ANGÓS
SPECIALIST. DIGESTIVE DEPARTMENT

Intestinal diverticula are small bags or sacks that protrude from the light of the intestine to the outside of the intestine. They are most often found in an area of the left colon called the sigma.
The term diverticulosis refers to the existence of diverticula in the colon. And we speak of diverticulitis when any of these diverticula become inflamed.
Most colon diverticula are produced by an increase in the internal pressure of the colon. This causes, over the years, its internal layers (mucosa and submucosa) to herniate or prolapse through the weakest and least resistant points of the wall, giving rise to the appearance of diverticula.
The less fiber we take in with our diet, the greater the pressure inside the colon and the more frequent the appearance of the diverticula.

What are the symptoms of diverticulosis and diverticulitis?
More than 80% of people with diverticulosis are asymptomatic. In those who appear symptoms, they are due to the motor alterations of the colon (hypertonia) and are presented in the form of continuous or intermittent abdominal pain, normally located in the lower left part of the abdomen (iliac fossa), where the sigma is located. It is usually relieved by evacuation and/or expulsion of gases.
Patients with diverticulitis usually present with acute, constant pain, usually located in the left iliac fossa (this is why it is called "left-sided appendicitis"), with irradiation towards the back, fever accompanied by shrapnel and, sometimes, change in intestinal rhythm, from diarrhea to constipation. Nausea, vomiting, fatigue and abdominal distension may also occur.
The most common symptoms are:
- Abdominal pain.
- Fever.
- Change of intestinal rhythm.
- Nausea.
Do you have any of these symptoms?
You may have diverticulum in your colon
How is diverticulosis diagnosed?
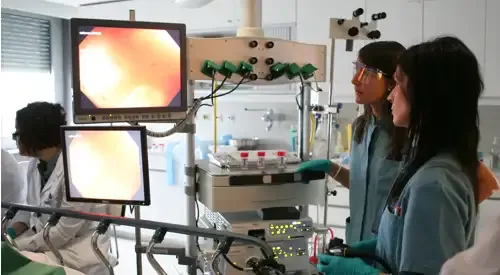
To confirm the suspected diagnosis of diverticulosis and given the need to rule out other more serious organic diseases with similar symptoms, such as colon cancer, we must perform radiological and/or endoscopic exams, such as a barium enema or colonoscopy.
In view of the clinical suspicion of diverticulitis, the most reliable and safe diagnostic methods are computerized axial tomography (CT) and ultrasound.
When the acute phase of inflammation has passed, it is advisable to perform a colonoscopy to confirm the diagnosis and rule out other processes.
How are diverticulosis and diverticulitis treated?
Treatment of diverticulosis should aim to relieve symptoms and prevent complications.
Generally, a diet rich in vegetable fiber with bran supplements and other laxatives that provide fiber alleviates abdominal pain, controls bowel movements, avoiding bowel movements, and reduces abdominal distension.
Antispasmodic drugs that act selectively on the colon muscles improve pain by inhibiting sigma contractions. If these drugs are not enough, analgesics (pentazocine type) can be used, which, in addition to calming the pain, reduce the pressure inside the colon.
Surgery will be resorted to, although not urgently, when episodes of diverticulosis are repeated frequently, fistulas and/or intestinal subocclusions appear.
Diverticulitis should be treated, initially, by bed rest, absolute diet, intravenous hydration, analgesics and intravenous antibiotics.
If there are signs of intestinal obstruction (nausea, vomiting and marked abdominal distention), a nasogastric tube will be placed to decompress the intestine.
When a perforation of the diverticulum occurs with peritonitis, an abscess is formed or a fistula is produced towards a neighboring organ, the treatment will be surgery, resecting the affected segment of colon with drainage of the abscess and a temporary colostomy bag that will be closed in a few months.
The Department of Digestive
of the Clínica Universidad de Navarra
The Digestive Department of the Clinica Universidad de Navarra is composed of a multidisciplinary team of specialists who are experts in the diagnosis and treatment of diseases of the digestive tract.
Our objective is that each diagnosis be carefully established and the treatment plan adjusted to each patient.

Why at the Clinica?
- Medical specialists who are national references.
- Specialized nursing team.
- Endoscopy Unit and High Risk Digestive Tumor Prevention and Consultation Unit to offer the best care to our patients.















