Gastrointestinal bleeding
"The diagnosis of digestive hemorrhage is very simple and many times the patient does it himself when he sees blood or mane in the stool".
DR. Mª TERESA BETÉS
SPECIALIST. DIGESTIVE DEPARTMENT

Gastrointestinal bleeding is the loss of blood from the digestive tract. According to its evolution, this loss can be acute or chronic, depending on the volume of blood lost and the time it has been lost.
According to their origin, they are classified as high or low digestive hemorrhage. High hemorrhages are those that originate in the esophagus, stomach and duodenum, and low hemorrhages are those that originate in the rest of the small intestine and colon.
In general, the symptoms are characteristic and give no option to doubt. The biggest problem is to determine their origin and cause.
When there is a history of those described and the bleeding presents symptoms that give away its origin, the diagnosis is usually not difficult. However, some hemorrhages are a real headache for the specialist, the patient and his family, which requires multiple tests, one after another, without finding the cause in many cases.

What are the symptoms of GI bleeding?
The most important symptom of acute hemorrhage is the visualization of fresh, semi-digested or mane shaped blood in the belly.
A special type of stool that is composed of digested blood, and that presents a pasty and sticky aspect, shiny black (similar to tar), with a very peculiar foul smell like rotten meat, is called melenas. The darker, smelly and digested the blood is, it means that its origin is higher (stomach, duodenum, high portions of the small intestine).
If the blood is fresh, bright red and hardly smelling, it usually means that its origin is close to the anus. In some cases of high hemorrhage, especially if it is important or accompanied by vomiting, blood can be expelled by the mouth, either fresh or as coffee grounds (hematemesis).
Another frequent symptom is the increase of intestinal noises and a special sensation of "laziness" due to the sudden drop in blood pressure. In the most important cases, tachycardia, cold sweat, dizziness, loss of consciousness and even shock appear. If the hemorrhage is not controlled it can have a fatal outcome.
What are the most common symptoms?
- Visualization of fresh, semi-digested blood in the womb.
- Manes.
Fortunately, many digestive hemorrhages are self-limiting.
On many occasions, the only thing that alerts the doctor to the existence of a chronic hemorrhage is anemia with low iron in the blood.
These are usually well-tolerated anemias and are discovered by chance in routine tests, although in some cases the patient presents a sensation of unusual tiredness and pallor.
Do you have any of these symptoms?
You may have a digestive hemorrhage
What causes gastrointestinal bleeding?
The causes of upper gastrointestinal bleeding can be varied.
In order of frequency from highest to lowest: Gastric or duodenal ulcer, esophagogastric varicose veins, diffuse lesions of the internal lining of the stomach (gastric mucosa), tearing by intense vomiting of the union between the esophagus and the stomach (Mallory-Weiss syndrome), inflammation of the esophagus (esophagitis), hiatus hernia, tumors, etc.
The causes of lower gastrointestinal bleeding are also varied, and the lesions that produce it have different frequency of appearance according to the age of the patients.
In patients of a certain age, the two most frequent causes are diverticula in the colon and angiodysplasias in the small intestine or colon.
Large tumors and polyps of the colon are a rare cause of acute bleeding, and if they do occur, it is usually intermittent and not very large. However, they are a frequent cause of chronic bleeding that is unnoticeable, but produces anemia in the patient.
Although low digestive hemorrhages in children, adolescents and young adults are rare, there are entities that can produce them among which chronic inflammatory diseases of the intestine (ulcerative colitis and less frequently, "Crohn's disease"), and Meckel's diverticulum stand out.
There are other causes of high or low bleeding, both chronic and acute, such as infectious, other tumors, fistulas between blood vessels and the digestive tract, complication of endoscopic maneuvers, taking antiaggregant or anticoagulant and others.
How is the recovery from a digestive hemorrhage?
As already mentioned, many bleeds will stop on their own. However, it is essential to always go to an Emergency Department, since the outcome is unpredictable and some of its causes are serious diseases.
In general, the prognosis depends on two factors, on the one hand, the severity of the hemorrhage itself and on the other hand, the seriousness of the cause that produced it.
In cataclysmic hemorrhages, which cannot be controlled, the prognosis is fatal.
In hemorrhages that are controlled, the prognosis depends on the recurrence of the hemorrhage and the adequate treatment of the cause that produced it.
Today, treatments to stop the bleeding, if localized, are effective.
Bad prognostic factors are that the bleeding is massive, persistent or repeated, the patient is very affected by the volume of blood lost (very low blood pressure, unconscious ...), which has other associated debilitating diseases (heart failure, respiratory, liver, advanced tumors ...), which occurs in esophageal or gastric varicose veins and that is over 60 years, among others.
How is GI bleeding diagnosed?
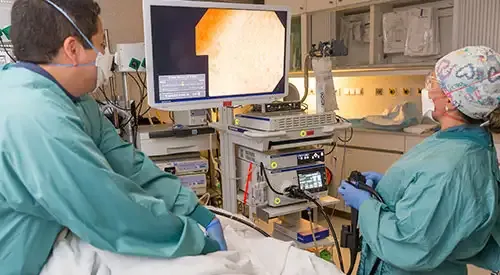
When bleeding occurs at a point in the digestive tract that is accessible to gastroscopy or colonoscopy (esophagus, stomach, duodenum, colon or last portion of small intestine), these are the most useful method. An endoscopy will, in most cases, pinpoint the point of the bleeding, establish its cause and, on many occasions, will serve to apply an effective treatment to cut it.
In the event that the gastroscopy and colonoscopy do not provide information about the origin of the bleeding (approximately 5% of the time), an exploration of the entire small intestine is carried out using the endoscopic capsule.
When the diagnosis is not reached by endoscopy, other techniques that help are arteriography (catheterization of arteries and veins of the abdomen), scintigraphy with marked red blood cells, radiological study of the digestive tract with barium meal, the scanner and in extreme cases, surgical exploration.
In any case, in the event of acute or chronic bleeding, all diagnostic possibilities must always be exhausted given the high risk they present and the seriousness of some of their causes.
How is digestive bleeding treated?
Always, in case of suspicion of acute or chronic digestive bleeding, one must go to the doctor.
If the hemorrhage is acute, the appropriate thing to do is to go to an emergency service. It should be the specialist in the digestive system who studies the patient and indicates the treatment. Overlooking these processes is reckless, as some will require urgent treatment and others an accurate diagnosis given their severity.
The treatment of acute hemorrhages has several steps that consist of placing the patient with an IV through which serum or blood will be administered to replace the lost volume, stabilizing the patient if possible, performing an upper endoscopy (gastroscopy) or lower endoscopy (colonoscopy), or both if necessary, -if the point of hemorrhage is located, it will be treated by endoscopic methods (coagulation, injection of vasoconstrictors and sclerosants, ligation. ...), administration by vein of drugs that block the manufacture of acid by the stomach and even vasoconstrictors, admission of the patient and control of their progress.
If the diagnosis is not reached by endoscopy and the bleeding is heavy, an arteriogram must be performed to locate the point of bleeding and try to plug it up.
In some cases surgery may be necessary if the bleeding is not stopped or the point that produces it is not located.
The treatment of chronic bleeding is to diagnose its cause and put an appropriate treatment, since in many cases are important causes that can produce them (tumors).
The Department of Digestive
of the Clínica Universidad de Navarra
The Digestive Department of the Clinica Universidad de Navarra is composed of a multidisciplinary team of specialists who are experts in the diagnosis and treatment of diseases of the digestive tract.
Our objective is that each diagnosis be carefully established and the treatment plan adjusted to each patient.

Why at the Clinica?
- Medical specialists who are national references.
- Specialized nursing team.
- Endoscopy Unit and High Risk Digestive Tumor Prevention and Consultation Unit to offer the best care to our patients.















