Heart failure
"The feeling of shortness of breath during physical exercise is the main symptom".
DR. JUAN JOSÉ GAVIRA
SPECIALIST. CARDIOLOGY DEPARTMENT

Heart failure causes the heart to lose the ability to maintain that adequate flow, even at the expense of increasing pressures.
The Clinic's Department of Cardiology and Cardiac Surgery is a reference center in the treatment of heart failure.
We have extensive experience and the latest technology for the diagnosis and treatment of this pathology.
We are experts in procedures such as slow ultrafiltration, to remove excess water that accumulates as a result of heart failure, coronary angioplasty or the implantation of a special cardiac pacemaker.
In the most serious cases in which other treatments have not been effective, a heart transplant is necessary. With the incorporation of new surgical techniques and immunosuppressive drugs, the results have been improved and we currently offer a survival rate of 90% per year and 75% after five years.
We have research lines open to evaluate the usefulness of implanting myocytes (contractile heart cells) obtained from adult stem cells.

What are the symptoms of heart failure?
The main symptoms caused by heart failure are those derived from
- A decrease in the supply of oxygen to the tissues, due to a decrease in cardiac output.
- Compensatory mechanisms, which tend to increase intravascular pressures and cause symptoms of congestion.
- The universal symptom of heart failure is dyspnea or "shortness of breath", which becomes evident during physical exercise or, in more severe cases, at rest (resting dyspnea), with the position of decubitus (orthopnea) or suddenly at night (paroxysmal nocturnal dyspnea).
Other very suggestive symptoms of heart failure, in this case right, are the edema in declining parts (exaggerated swelling in ankles and/or pretibial region) and the sensation of abdominal swelling (hepatomegaly or ascites).
The most common symptoms are:
- Shortness of breath (dyspnea).
- Dyspnea at rest and in decubitus (orthopnea).
- Choking sensation that worsens at night (paroxysmal nocturnal dyspnea)
- Swelling of the ankles (edema).
- Fatigue.
Do you have any of these symptoms?
You may have heart failure
What are the causes of heart failure?
Heart failure occurs when there is a disorder of the heart muscle, when the heart is overburdened, or when there is a combination of these two factors.
The disorders that most frequently lead to heart failure include ischemic heart disease (myocardial infarction), high blood pressure, cardiomyopathies, valve diseases, some congenital heart diseases and, more rarely, diseases of the pericardium.
Less frequently, heart failure is due to extracardiac disorders, such as hyperthyroidism or severe anemia.
How is heart failure classified?
The stages of heart failure have an important prognostic value and are used as a decisive criterion in the choice of treatment, especially for certain therapeutic interventions, both medical and surgical.
- Stage 1. Patients at risk of heart failure without symptoms.
- Stage 2. Patients with heart disease without symptoms.
- Stage 3. Patients with heart disease with symptoms.
- Stage 4. Patients with severe heart disease with symptoms.
How is heart failure diagnosed?
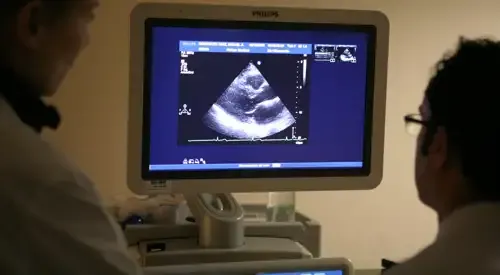
It is essential to correctly diagnose the cause in order to establish the most appropriate treatment.
The diagnosis of heart failure is made by the physician in consultation, usually based on relatively simple clinical criteria.
However, just as important as the diagnosis of heart failure is the cause that is causing it, since on many occasions this is reversible. For this purpose, other more sophisticated examinations are usually used:
The echocardiogram confirms the ventricular dysfunction and attempts the diagnosis of the casual heart disease.
With a simple chest X-ray the cardiac silhouette and the lung fields are evaluated.
By means of a blood and urine analysis, renal function, ions, glycaemia, hemogram, as well as proteinemia and proteinuria in case of edema are studied.
CT and MRI help determine the cause by detecting, for example, stenosis in the coronary arteries.
How is heart failure treated?
Once heart failure has been diagnosed, the correct treatment must take place.
Initially, medical-pharmacological measures are applied, of which the Clinic is incorporating the latest advances.
Rehabilitation, through physical exercise, in addition to being a preventive measure, is very useful for patients affected by this syndrome.
The Clinic also contemplates the treatment and domiciliary control of the patient.
Depending on the response to medical treatment and the prognosis of the heart failure, other treatments may be applied.
It is indicated to improve heart muscle irrigation in patients with ischemic cardiomyopathy. Various techniques are used for this purpose:
- Interventional cardiology techniques, such as angioplasty and stenting, atherectomy or guided dilation with intracoronary ultrasound.
- Surgical revascularization. Aortocoronary bypass surgery can be performed without extracorporeal circulation and complete revascularizations can be performed with arterial grafts (mammary and radial arteries). This reduces the aggressiveness of surgery and hospitalization and improves long-term results.
- In patients without technical possibilities of revascularization due to poor quality of the coronary arteries, the intramyocardial laser creates channels that tend to form new vessels.
At the Clinica Universidad de Navarra we are carrying out experimental studies with genes that can increase the vessels generated by the laser or encourage the synthesis of proteins that intervene in the contraction of the heart.
Mechanical assistance, also called circulatory or ventricular assistance, is a mechanical device composed of a hydraulic propulsion system that, when connected to the circulatory system, is capable of replacing cardiac function either temporarily or permanently.
The Clínica Universidad de Navarra began its mechanical assistance program in 1992. At present, we have various ventricular assistance devices, which allow us to perform ventricular assistance in situations of acute ventricular failure, as a bridge to heart transplantation and as definitive assistance.
These devices require a surgical team with sufficient experience, since their implantation is usually done in complex patients with multiple associated pathologies. On the other hand, its postoperative management requires a multidisciplinary team to solve the possible complications that may arise.
At the Clinica Universidad de Navarra we have a multi-disciplinary team of experts in ventricular assistance (surgeons, anesthesiologists, hematologists, infectious diseases).
In addition, we have nurses who are highly specialized in the handling of these devices, who in a coordinated manner control these patients daily until they are discharged.
With the incorporation of new surgical techniques and immunosuppressive drugs, the results have been improved and we currently offer a survival rate of 90% per year and 75% after five years.
The Clinic was the second hospital in Spain to perform heart transplantation in 1984 and the first to perform cardiopulmonary transplantation in 1986.
Likewise, hospital stays have been reduced to 7-10 days, with the consequent reduction in costs and post-operative complications.
What clinical trials do we have on insuficiencia cardíaca?
The Department of Cardiology
of the Clínica Universidad de Navarra
The Department of Cardiology of the Clinica Universidad de Navarra is a center of reference in different diagnostic techniques and coronary treatments.
We have been the first center in Europe to place a pacemaker by means of a catheterization without the need to open the chest, for cases of severe heart failure.
The Cardiology Department of the Clinic collaborates with the Radiology and Cardiac Surgery Departments to achieve a quick and precise diagnosis of the patient.

Why at the Clinica?
- Specialized Arrhythmia Unit of national reference.
- Unit of Hemodynamics and Interventionist Cardiology equipped with the best technology.
- Cardiac Imaging Unit to achieve the highest diagnostic accuracy.


















