Pericarditis
"If detected early and with proper treatment, patients achieve full recovery in less than a month".
DR. MANUEL GARCÍA DE YÉBENES
PERSON IN CHARGE. CARDIOLOGY DEPARTMENT

Pericarditis is the inflammation of a double membrane that surrounds the heart, called the pericardium.
It can lead to pericardial effusion (the formation of fluid between the membrane that is attached to the heart and that which is in contact with the lungs) and can also lead to thickening, retraction, and calcification of the pericardium.
Pericardial effusion puts pressure on the heart and restricts the pumping action.
The prognosis is good in most cases and symptoms usually disappear within a few days with proper treatment.
This treatment should be followed for 2-3 weeks, even if the patient is already well.
Although it may reappear in 15-30% of cases, recurrences are usually benign and leave no after-effects.

What are the symptoms of pericarditis?
Acute pericarditis is characterized by symptoms due to inflammation of the pericardium: center-thoracic pain that is usually acute and may radiate to the back, neck, arms, and left shoulder (sometimes radiating to the right arm or both).
The pain is accentuated when the patient is lying on his back and decreases when sitting and leaning forward. It also increases with deep breathing, which makes breathing difficult.
Some patients have a fixed discomfort at the level of the sternum that resembles the pain of an acute myocardial infarction. The pain may be accompanied by fever, rapid heartbeat, coughing and pain when swallowing and usually lasts for several days.
Other symptoms appear when there is pericardial effusion, especially if it is abundant and occurs in a short time (there may be difficulty breathing, dizziness, etc).
Unlike the pain of angina, the pain of pericarditis is not related to physical exercise.
Most common symptoms:
- Center-thoracic pain.
- Fever.
- Tachycardia.
- Cough.
- Pain when swallowing.
Do you have any of these symptoms?
You may have pericarditis
Constrictive pericarditis
It consists of an increase in the thickness and rigidity of the pericardium, which stops being an elastic membrane to become rigid. It is a typically chronic process with some variations.
It is estimated that about 2% of patients who have suffered acute pericarditis, over time, present a constrictive pericarditis.
The least frequent cause is idiopathic or viral and the most frequent causes are tuberculous and purulent. The most frequent symptoms are: fluid retention (which begins to manifest itself by swelling of the ankles) and excessive tiredness when doing physical exercise.
The symptoms of constrictive pericarditis are usually permanent and progressive until the patient is treated surgically with pericardium extraction or pericardiectomy.
Only in a minority of patients, the constriction can be transient and reversible, so one can wait 2-3 months with conservative treatment before practicing surgery.
Recurrent pericarditis
Approximately 15-30% of patients with acute pericarditis have recurrences (another similar episode after a while) or persistence of the initial episode, often accompanied by effusion or pericardial effusion. This risk is lower in idiopathic pericarditis and when colchicine is administered from the beginning.
Recurrent pericarditis manifests itself as a recurrence of the symptoms of acute pericarditis. However, the predominant symptom is usually chest pain, without other clinical manifestations. The term recurrent pericarditis refers to the syndrome in which acute pericarditis recurs after the agent that caused the initial episode has disappeared or has ceased to be active.
Recurrence of symptoms can occur at any stage after the symptoms of initial pericarditis have disappeared but usually occurs more than six weeks after the initial episode.
When the symptoms of the first episode are persistent or unabated within the first six weeks of evolution, it is called "incessant pericarditis," rather than recurrent.
How is pericarditis diagnosed?
The doctor has three diagnostic criteria in acute pericarditis, which are not necessarily present at the same time: the medical history of typical pain (often accompanied by fever), cardiac auscultation and electrocardiogram abnormalities.
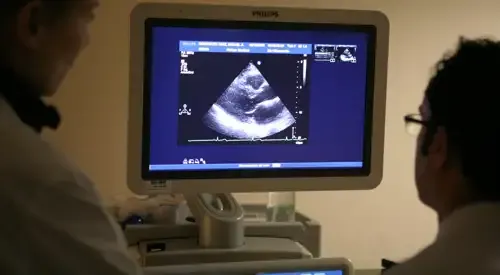
There is a fourth criterion that is presented with lesser counts and is the increase in fluid between the two layers of the pericardium. This is called pericardial effusion and can be seen by performing an echocardiogram.
Generally, it is enough to make the diagnosis that two of these three criteria are present at some point in the evolution of the disease.
A sample of fluid can be taken from the pericardium using a needle. This procedure is called pericardiocentesis.
The extracted fluid sample is analyzed in order to detect the presence of an infection or other diseases, but in most cases of acute pericarditis it is not necessary to perform pericardiocentesis for its diagnosis, since it is a benign process that tends to remit in a short time.
How is pericarditis treated?
Most often, acute pericarditis is idiopathic (cause unknown). It is not considered necessary to make studies to know the cause, since most of the times the clinical course is benign and the patients improve with unspecific measures: rest while the pain lasts, besides nonsteroidal anti-inflammatory (ibuprofen or aspirin), in high doses during 2-3 weeks. Colchicine can also be administered as it reduces the risk of recurrence.
Other possible causes are the following: infection (most of the cases by virus), radiation, thoracic trauma, drugs, toxins, metabolic alterations (the most frequent is renal failure), tumors, rheumatic diseases, inflammatory gastrointestinal diseases.
The goal of treatment is twofold: to relieve pain and to reduce inflammation of the pericardium. If pericarditis is secondary to another disease, the causative disease must be treated at the same time.
In those that produce significant pericardial effusion, a pericardial puncture may be necessary to remove the effusion.
The Department of Cardiology
of the Clínica Universidad de Navarra
The Department of Cardiology of the Clinica Universidad de Navarra is a center of reference in different diagnostic techniques and coronary treatments.
We have been the first center in Europe to place a pacemaker by means of a catheterization without the need to open the chest, for cases of severe heart failure.
The Cardiology Department of the Clinic collaborates with the Radiology and Cardiac Surgery Departments to achieve a quick and precise diagnosis of the patient.

Why at the Clinica?
- Specialized Arrhythmia Unit of national reference.
- Unit of Hemodynamics and Interventionist Cardiology equipped with the best technology.
- Cardiac Imaging Unit to achieve the highest diagnostic accuracy.


















