Trigeminal neuralgia
"An adequate neurological evaluation is very important to distinguish it from other types of craniofacial pain".
DR. PABLO IRIMIA
SPECIALIST. NEUROLOGY DEPARTMENT

What is trigeminal neuralgia?
Trigeminal neuralgia is a disorder of the trigeminal nerve or cranial nerve V that causes recurrent episodes of paroxysmal pain (intense, sharp, superficial, stabbing or electric), in one half of the face.
It usually lasts of a second to two minutes and generally it respects the dream.
It is considered the most painful affliction known in the medical practice. The right side usually is affected more frequently (60%), being bilateral in only 1-6% of the cases.
Frequently, the pharmacological treatment is not effective and requires surgical treatment.
At the Clínica Universidad de Navarra we have neurosurgeons who are experienced in the application of the different surgical alternatives.

What are the symptoms of trigeminal neuralgia?
Although pain can occur spontaneously, it is common to have trigger zones that are activated by tactile or thermal stimuli (chewing, talking, combing your hair, brushing your teeth, eating or yawning), daily activities that can trigger a very disabling pain crisis.
The most common symptoms are:
- Severe paroxysmal pain in the middle of the face
Do you have any of these symptoms?
You may have trigeminal neuralgia
What are the causes of trigeminal neuralgia?
The origin of this clinical picture is usually unknown (idiopathic). Peripheral and central causes can be distinguished. It has been associated with irritation of the trigeminal nerve because a vessel (artery or vein) is compressed or very rarely because of compression due to a tumor (0.8-3% of total cases).
1-2% of patients with multiple sclerosis (demyelinating disease of the nervous system) develop trigeminal neuralgia, which accounts for 2-3% of trigeminal neuralgias.
What is the prognosis of trigeminal neuralgia?
Overall, 80-85% of patients are pain-free in the long term with medical treatment.
Among those who do not improve, there are different radiofrequency procedures and surgical techniques that relieve and even cure the symptoms in a high percentage of patients.
With radiosurgery, pain relief is not immediate, occurring in about 3 weeks. About 53% of the patients achieve a disappearance of the pain and another 35% achieve a significant reduction.
How is trigeminal neuralgia diagnosed?
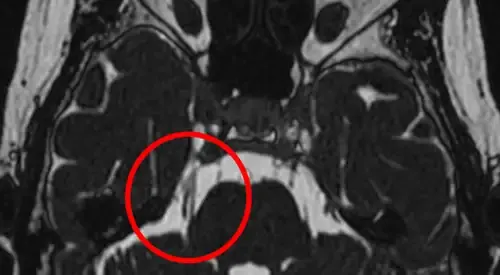
The diagnosis of trigeminal neuralgia is based primarily on the clinical symptoms reported by the patient (location of pain, time of onset, triggers, pain-free intervals, medication) and on physical examination (facial sensory evaluation, corneal reflex, evaluation of chewing muscles).
Although neuroimaging studies are normal in most cases, high field magnetic resonance imaging (MRI) allows observation of vascular loops and vessel compression over the trigeminal nerve that in conventional MRI studies usually go unnoticed, in addition to ruling out tumors, demyelinating diseases, etc.
How is trigeminal neuralgia treated?
Conservative pharmacological treatment is the first therapeutic option.
Some anticonvulsants, such as carbamazepine, gabapentin, phenytoin and lamotrigine, have been shown to reduce or control pain.
Other medications, such as baclofen, pimozide, tizanidine, tocainide, clomipramine, or amitriptyline, may have some effectiveness in some cases. The habitual analgesics (aspirin, paracetamol, etc) are not usually useful to control the pain.
Unfortunately, it is not always fully effective and non-pharmacological treatments such as microvascular decompression or retrogasserian thermocoagulation are necessary.
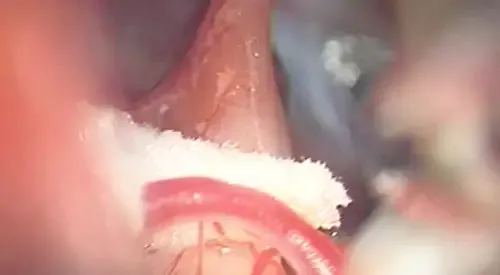
When pain control is not achieved conservatively, the non-pharmacological treatment that is being used more and more often is microvascular decompression (DMV or Janetta's technique). If we can objectify a compression through an MRI study, this surgical approach can be indicated with a high and permanent degree of success.
The approach used is a retro-sigmoid craniotomy, through which the site of the compression is sought. After a meticulous microscopic dissection of the subarachnoid, an insulating material is placed (which in these cases is usually Teflon), so that the heartbeat, pulsation or vascular movement is not transmitted to the trigeminal nerve on that side and that the irritation of the same, and with it the pain, is reduced. It is performed under general anesthesia and lasts between 2 and 3 hours.
This same procedure can be performed, although less frequently, for other cranial compression neuropathies.
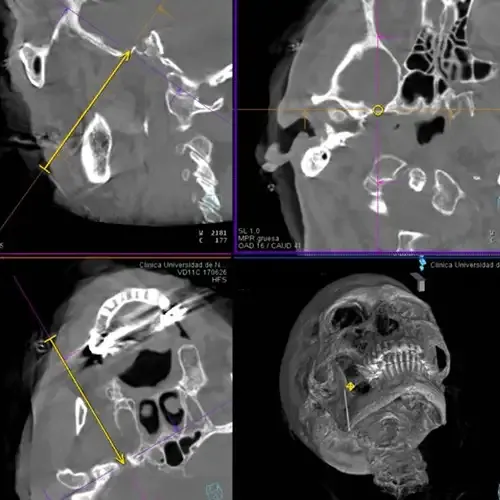
In the event that no compression of the V par is observed, the surgery is partially effective or a pre-anesthetic assessment of the patient contraindicates that intervention, a retrogasserian thermocoagulation or percutaneous radiofrequency trigeminal rhizotomy (PRT) can be performed.
Its objective is to selectively destroy the pain fibers (nociceptive). To do this, special surgical facilities are used to obtain radiological images and 3-dimensional (3D) reconstructions that give us more security when performing this approach.
This procedure consists in introducing a needle through the cheek to the oval hole, which is the entry point to the cavum or Meckel's fossa, where the Gasser's ganglion, crescent or trigeminal ganglion is located. The aim is to produce an injury by thermocoagulation of the affected branch(s) and to reduce pain.
This technique is less aggressive than the first and is performed under local anesthesia with sedation and lasts approximately 30 minutes, and the patient is discharged in 12 or 24 hours.
The Department of Neurosurgery
at the Clínica Universidad de Navarra
The Neurosurgery Department has specialists with a great deal of experience in care and research and the most advanced technology.
We are the first Spanish center that incorporates high field intraoperative magnetic resonance (3T). This allows the maximum precision and control in cranial surgery.
We are the Spanish medical center with the most experience in Parkinson's surgery by means of deep brain stimulation. We have the latest technology with localized ultrasound (HIFU) and extensive experience in treating essential tremor and Parkinson's disease without an incision.
Treatments we perform
- Alterations in the circulation of the cerebrospinal fluid
- Infusion Pumps
- Epilepsy Surgery
- Deep brain stimulation
- HIFU, high intensity ultrasound
- Trigeminal Neuralgia
- Pediatric Neurosurgery
- Neuronavigation of the spine
- Spine Pathology
- Brain Tumors
- Pituitary Tumors

Why in Navarre?
- The first Spanish center with a high field intraoperative magnetic resonance (3T).
- Precision and minimally invasive surgery.
- Experts in the use of HIFU for the treatment of tremor.




