Uterine Fibroids
"Radiofrequency ablation of fibroids is a novel treatment with fantastic short- and long-term results."
DR. ÁLVARO RUIZ
SPECIALIST. GYNAECOLOGY AND OBSTETRICS DEPARTMENT

What are uterine fibroids?
Uterine fibroids are the most common tumors of the female genital tract and probably the most common benign tumor in women.
They originate from uterine smooth muscle and are often asymptomatic. In 25% of cases they produce symptoms depending on their location or size, such as abnormal uterine bleeding, symptoms due to compression of neighboring structures, pelvic pain or infertility.
In small and asymptomatic myomas, expectant management (evolutionary control) can be chosen, as long as women remain asymptomatic and no exaggerated growth of the myoma is observed.
In patients close to the age of menopause and asymptomatic, we should also consider expectant management even with some independence of the size of the myoma, since after menopause it is normal to observe a decrease in size or even degeneration of the myoma.
Radiofrequency ablation is a recent alternative for minimally invasive treatment of myomas. This technique is routinely used in the Clinica, with excellent results in the short and long term.

What are the symptoms of uterine fibroids?
About 50-80% of fibroids are asymptomatic. The symptoms that can be found are:
- Uterine bleeding. This is the most frequent symptom (62%). It usually occurs in the form of heavy menstruation (menorrhagia) and is typically associated with submucous fibroids.
- Pain. It may be due to torsion, cervical dilatation (parido myoma), myoma degeneration or nerve compression.
- Symptoms due to extrinsic compression. Urinary symptoms due to bladder compression or constipation due to intestinal compression.
- Increased abdominal volume.
- Anemia.
- Infertility. The myoma can prevent fertilization or implantation due to its location in the uterus (tubal obstruction or alteration of the normal anatomy).
Twenty percent of fibroids grow during pregnancy and return to normal after delivery, and degeneration or necrosis is common.
The risk of miscarriage may increase in those who deform the morphology of the cavity and the incidence of preterm delivery or problems in childbirth depending on the location of the myoma.
The most common symptoms are:
- Abnormal uterine bleeding.
- Pelvic or lower abdominal pain.
- Extrinsic compression symptoms.
- Infertility
Do you have any of these symptoms?
You may have a uterine fibroid
What are the causes of uterine fibroids?
The cause of fibroids is unknown, although it is accepted that it is a tumor derived from uterine smooth muscle and rarely malignant.
It appears that the hormones of the menstrual cycle (estrogens and progesterone) actively influence the growth of fibroids. Also other substances, such as growth factors and other hormones have an influence on the development of the endometrium, acting synergistically with progesterone or favoring its activity. All this could provoke the genetic alteration that would lead to the disproportionate growth of a group of cells that would form a myoma.
Who can suffer from it?
The incidence in the general population is 25%, but we know that this is a clinical datum that probably underestimates the real frequency, which may exceed 50%.
It is most often diagnosed in the third and fourth decades of life and in addition to black race, family history, early menarche (first menstrual period), obesity or red meat are considered risk factors.
On the other hand, a protective relationship has been found in multiparity (having several children), smoking and the intake of foods of vegetable origin.
The absence of menstrual cycles for any reason (such as pregnancy) also seems to have a favorable influence.
Can a uterine fibroid become malignant?
Several histological subtypes have been identified, although macroscopically there are no differences between them. According to their location they are distinguished:
- Subserosal myomas: located in the outermost part of the uterus, under the most superficial layer, which is called the visceral or serous peritoneum. They can reach a large size and are not very symptomatic.
- Intramural myomas: these are the most frequent (55%) and proliferate in the muscular layer of the uterus, which is called the myometrium.
- Submucosal myomas: they protrude to a greater or lesser extent into the endometrium (innermost layer), towards the uterine cavity. They are the most symptomatic (especially bleeding).
When the growth is disproportionate to the irrigation of the myoma, it can undergo degeneration processes, most of the time without transcendence (hyaline -65%-, cystic -4%-, myxomatous -15%-, calcification -10%-, fatty, necrosis and malignant or sarcomatous -0.5%-).
Although myomas are benign tumors, as has been explained, statistics indicate that approximately one in every 10,000 patients with myomas will present a malignant tumor (called leiomyosarcoma), probably due to an initial misdiagnosis. In these cases the growth of the myoma is usually rapid and shows signs of abnormal vascularization. This possibility should be kept in mind especially in post-menopausal patients.
How are uterine fibroids diagnosed?
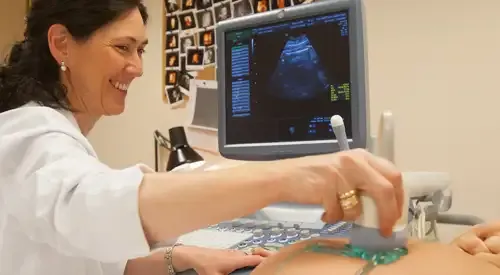
However, ultrasound is the imaging test that offers the best performance in the diagnosis of fibroids, especially transvaginal ultrasound, which allows greater detail in the exploration.
Other techniques can also be used to confirm or clarify the diagnosis in some circumstances, such as diagnostic hysteroscopy, hysterosalpingography or sonohysterography, or even magnetic resonance imaging, but this is not common.
How are uterine fibroids treated?
In case of enlargement or appearance of symptoms, treatment (medical or surgical) may be indicated at any time.
Hormonal drugs can be used.
Classically, GnRH analogs have been used, showing a decrease in myoma size and bleeding. They have an important limitation in the side effects, since they cause a pharmacological menopause, with identical symptoms, and with long-term use even osteoporosis. Also a major limitation to their widespread use is the fact that after treatment the size increases again within 4-6 months. This same medication can be used in patients who are candidates for surgery during the months prior to surgery in order to reduce the size of the myoma and to recover the possible anemia of symptomatic patients, or even in perimenopausal and symptomatic patients to avoid surgery, but this is very infrequent.
Other medical (hormonal) treatments could be antiprogestagens (Mifepristone), with the consequent risk of endometrial hyperplasia, or the progesterone-releasing IUD, which in women with symptomatic uterine myomatosis (menorrhagia) manages to reduce uterine bleeding in a high percentage of cases, although it is not always possible to use it. Ulipristal acetate (Esmya) also manages to reduce the symptoms of bleeding and effectively reduces the size of the fibroids, although it requires frequent analytical control due to hepatic risk and when discontinued, the fibroids also increase in size again within a few months. This last drug can be used chronically to avoid surgery or as a preparatory treatment for surgery.
The definitive treatment of this pathology is surgical, and the different treatment options are based fundamentally on the location of the fibroids and the desire for gestation. There are two options:
Myomectomy
Only excision of the fibroids is carried out, preserving the uterus, which is repaired by closing the fibroids that have been removed. It is usually performed in women who wish to have children or in those who want to keep the uterus for any other reason. In this surgery the fibroids that have been previously seen and/or that are seen or palpated during the surgery are removed, which does not exclude the possibility that others may reappear in the future.
Hysterectomy
This surgery consists of completely removing the uterus, and is considered a definitive treatment.
Both techniques can be performed by open abdominal (conventional surgery in which the abdomen is opened generally below the pubic hairline), vaginal or laparoscopic (minimally invasive surgery, accessing the abdominal cavity through the vagina or through small holes in the abdomen). The location or size of the fibroids may determine in some cases the technique of choice.
Classically there has been some controversy regarding the choice of the best surgical treatment, with myomectomy raising doubts due to the risk of greater blood loss; however, several current scientific articles contradict this belief. In our center we routinely perform this technique, being possible to preserve the uterus in 99% of cases that the woman so desires and without significant complications during surgery.
It is also common to treat submucosal fibroids by hysteroscopic resection, vaginally, resecting only the fibroid that causes abnormal uterine bleeding and / or in some cases infertility. This technique consists of introducing a small camera (hysteroscope) into the uterine cavity and performing the excision of the myoma from inside the cavity. It is also performed in the operating room, under general or regional anesthesia, and recovery is very fast and tolerable, usually being an outpatient surgery.
Other possible treatment techniques would be embolization of the arteries supplying the fibroids or the uterine arteries (which supply the uterus), producing necrosis of the fibroids; or MRI-guided ultrasound, which is not recommended in women with reproductive desires due to the lack of data from long-term studies on its safety.
Their main advantage is that they are minimally invasive techniques that do not require aggressive interventions and can be performed on an outpatient basis. They are techniques with good results, but should be restricted to certain patients, as they have a higher rate of complications (mainly postoperative pain) and recurrences.
Finally, radiofrequency ablation is a recent alternative for the minimally invasive treatment of fibroids, and is currently presented as a real alternative that improves in many aspects the existing minimally invasive techniques for the treatment of fibroids. This technique is routinely used in the Clinica, with excellent results in the short and long term.
It requires ultrasound-guided puncture of the myoma to thermocoagulate the tissue in a controlled manner with a fine needle from the inside. This technique also does not require hospital admission and does not present serious complications, also allowing a rapid recovery of patients.
The Department of Gynecology and Obstetrics of the
of the Clínica Universidad de Navarra
Comprehensive care that includes a wide range of consultation and treatment options from regular preventive screening to the most advanced diagnostic and treatment options for obstetric and gynecological problems at all ages.
The department also offers routine pregnancy monitoring that includes a variety of diagnostic and screening procedures to identify potential problems of the fetus as well as its proper growth and development.
Diseases we treat
- Gynecological Cancer
- Prenatal diagnosis
- Endometriosis
- Urinary and fecal incontinence
- Masas anexiales
- Menopause
- Polycystic ovary syndrome
- Uterine Myomas

Why at the Clinica?
- Highly specialized team of doctors, nurses and midwives.
- Reproduction and Fertility Unit.
- Pregnancy follow-up with a personalized delivery.
- All the comfort, with the guarantee and safety of a hospital with the most advanced equipment.

























