Alcoholic Hepatopathy
"The disease is cured by abandoning alcohol, although in some cases a liver transplant is necessary".
DR. MERCEDES IÑARRAIRAEGUI
SPECIALIST. HEPATOLOGY UNIT

Alcoholic or ethylic liver disease is liver disease caused by excessive consumption of alcohol.
It is not a single clinical picture, but several modalities can occur depending on the amount of alcohol consumed, the time during which it is consumed and individual susceptibility.
There are three main types of alcohol-related liver disease, which are, from lesser to greater severity: alcoholic steatosis, alcoholic hepatitis, and ethylic cirrhosis.
The cause is excessive alcohol consumption. In general, it is considered that consumption of more than 80 grams of alcohol per day in men and 50 grams in women is harmful to the liver and may be sufficient for all the diseases mentioned in the previous section to appear over time.
One factor to take into account is the time of consumption. As a guideline, it is considered that an excessive amount of alcohol must be consumed for at least 5 years for serious liver damage to occur. Not all people who consume excessive amounts of alcohol develop serious liver disease. There is a component of individual susceptibility, as yet unidentified, that causes some people to develop cirrhosis and others only steatosis with the same intake of alcohol.

What are the symptoms of alcoholic hepatitis?
Steatosis is always asymptomatic.
Severe alcoholic hepatitis usually presents with symptoms of general illness such as tiredness, lack of appetite, digestive discomfort, pain in the right side of the abdomen and sometimes fever. In addition, more typical signs of liver disease can be observed as yellow skin color (jaundice), dark urine, accumulation of fluid in the abdomen (ascites) and clotting disorders, among others.
Cirrhosis may be asymptomatic in its early stages. Later it gives general symptoms or is manifested by its complications: yellow skin color (jaundice), digestive bleeding, accumulation of fluid in the abdomen (ascites), changes in behavior and level of consciousness and malnutrition, mainly. In addition, patients may have symptoms derived from alcohol toxicity in other organs.
What are the most common symptoms?
- Fatigue.
- Jaundice.
- Ascites.
Do you have any of these symptoms?
You may have an alcoholic liver disease
Ethylic Hepatic Steatosis
Ethylic Liver Steatosis is caused by the excessive ingestion of alcohol over a period of weeks and sometimes years. It consists of an accumulation of fat in the liver, as a result of the metabolic alterations produced by alcohol.
The patient has no symptoms, often goes through without analytical alterations and does not affect liver function. It is reversible with the cessation of alcohol consumption.
Some patients, even if they continue to consume alcohol, do not develop more serious forms of the disease while others evolve towards the other two conditions.
Alcoholic Hepatitis
Alcoholic Hepatitis is a subacute evolutionary picture. It is considered that excessive alcohol consumption must occur for at least 5 years to develop this condition. It is much more serious than steatosis.
The patient usually has symptoms, there are analytical liver disorders and liver function is affected.
The severity is variable. If alcohol consumption ceases, the disease can be cured, but there are patients who die and others who go on to the third type of picture.
Cirrhosis
The ethylic cirrhosis consists of the alteration of the liver structure by the scarring processes (fibrosis) produced in the liver by the effect of alcohol consumption, generally during many years. It is irreversible.
Although some patients are asymptomatic in the early stages of the disease, many have symptoms. Analytical alterations are produced and liver function deteriorates. Many patients end up dying as a result of the disease.
How is alcoholic liver disease diagnosed?
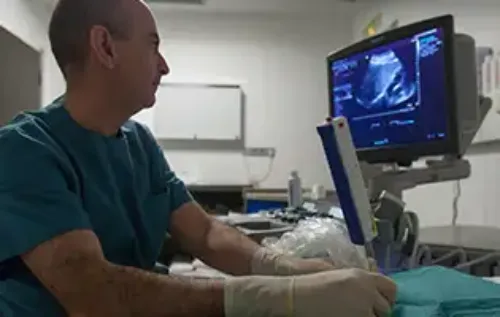
The doctor makes the diagnosis of alcoholic liver disease based on the history of alcohol consumption, physical examination, liver analysis, abdominal ultrasound and, in many cases, it is necessary to perform a liver biopsy to obtain the definitive diagnosis.
Many patients with alcohol-related liver damage, including steatosis, have elevated blood levels of a substance of hepatic origin, gamma-glutamyl-transpeptidase (GammaGT or GGT), which is the earliest biochemical marker of excessive alcohol consumption.
How is alcoholic liver disease treated?
The only effective treatment is to stop drinking alcohol. If there is alcohol dependency, stopping consumption requires psychiatric help.
The suppression of alcohol consumption allows the cure of steatosis and, in many cases, alcoholic hepatitis; when cirrhosis exists, it leads to an improvement in liver function, although cirrhosis is irreversible.
Depending on the degree of deterioration of liver function, these patients may later lead a normal life or, on the contrary, require a liver transplant to avoid death due to complications of cirrhosis.
The Hepatology Unit
of the Clínica Universidad de Navarra
We are pioneers in the application of gene therapy in the treatment of liver tumors and hereditary metabolic diseases, and we have extensive experience in the diagnosis and treatment of viral hepatitis and in the treatment of liver cancer using radioembolization systems with Ytrium-90 microspheres.
The Clinic is at the forefront in Spain in performing liver transplantation between living people.
Diseases we treat
Treatments we perform
- Hepatic Arterial Embolization
- Partial splenic embolization
- Genetic study in hepatology
- Liver Radiofrequency
- Liver Radioembolization
- Liver resection
- Liver transplantation

Why at the Clinica?
- Highly specialized team of professionals with more than 25 years of experience.
- Nursing team specialized in hepatic patients.
- Important research activity on the molecular mechanisms that cause some of these diseases.









