Haemodynamic and Interventional Cardiology
"We have the latest technology such as hybrid operating rooms that allow us to perform hemodynamic procedures with maximum precision and safety".
DR. RAFAEL RUIZ SALMERÓN PERSON IN CHARGE. HAEMODYNAMIC AND INTERVENTIONAL CARDIOLOGY UNIT

The Hemodynamics and Interventional Cardiology Unit of the Clinica Universidad de Navarra has the most advanced technology for the diagnosis and treatment of heart diseases, both at its headquarters in Pamplona and in Madrid.
The performance of catheterizations, in most patients by radial access (through an artery in the wrist), makes it possible to identify whether there are significant obstructions in the coronary arteries. If this is the case, we have the latest techniques to assess the need for implantation of pharmacoactive stents to solve the problem.
The Hemodynamics and Interventionist Cardiology Unit has a comprehensive program for the treatment of structural cardiopathies, which include valvular (TAVI implant - aortic valve), structural (closure of the permeable oval foramen, closure of the left ear) and congenital (interauricular communication, interventricular communication, persistent ductus arteriosus, coarctation of the aorta) pathologies.
The Interventional Cardiology Unit of the Clinica Universidad de Navarra, like the rest of the departments of the Clinic, offers personalized attention to the patient, with great efficacy and efficiency.
We do not have a waiting list for interventions, and they can be performed immediately after diagnosis or at the moment when the patient is most available.
Interventional cardiology treatment is less aggressive for the patient, with faster recovery, shorter admission time and fewer sequelae than heart surgery.

Cutting edge procedures with maximum security
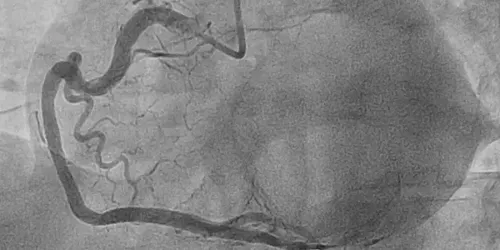
Percutaneous intervention of coronary artery lesions is today the mainstay of treatment of coronary disease.
The procedure consists of accessing with a catheter (very thin flexible tube), through a puncture in the radial or femoral artery, until reaching the origin of the coronary arteries in the aorta, next to the heart. Afterwards, the narrowed or obstructed areas are usually dilated with a small balloon, and then one or more stents are implanted to achieve an optimal result. The stent allows the obstruction to be prevented from reappearing in a percentage of more than 95% of injuries.
In some cases, when the disease in the coronary arteries is very serious, open heart surgery is used, but nowadays this is increasingly rare.
There are multiple types of stents (metal stents of various alloys), of different sizes and lengths to fit all lesions and arteries. All of them have an antiproliferative drug attached to them that inhibits the reaction of the artery to the implant, to prevent the obstruction from reproducing, and they are highly safe and effective.
In our center the success rate of the treated lesions is over 98%
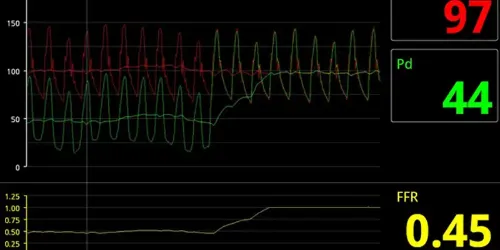
Pressure guiding is an invasive diagnostic technique that allows a very reliable assessment of the severity of the coronary lesions, in order to make decisions about which ones need a revascularization procedure.
Its use is simple because it is a very thin wire with a sensor at its distal end, which is introduced through a catheter into the coronary artery, beyond the area to be evaluated.
There are several similar techniques (FFR, iFR) that have demonstrated in important scientific studies their high diagnostic efficiency and excellent prognostic correlation, as endorsed by the European guidelines for coronary revascularization.
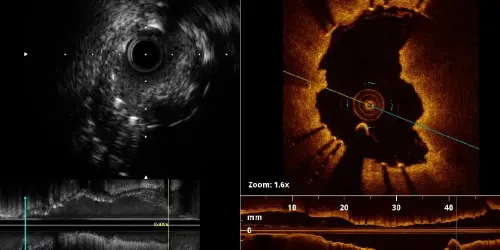
We have these two intracoronary imaging techniques, which allow us to assess very precisely the composition of the atheroma plate or the presence of anatomical situations that cannot be identified by angiography alone (coronary dissections, intracoronary hematomas, thrombus, aneurysms).
The resolution of the images obtained is of very high quality, even three-dimensional reconstructions are performed, and it also allows to confirm the adequate result of the interventions after the stent implantation.
They have proven to be very useful in the treatment of complex cases.
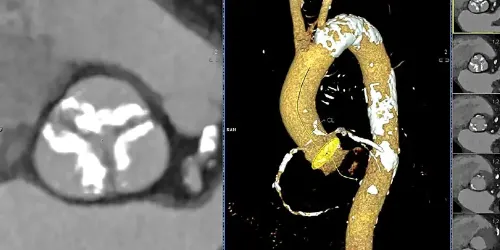
The results of this technique have proven to be superior to classic open surgery in many patients, especially those over 75 years old and those with other serious pathologies. It is even being used to treat previous prostheses that have degenerated.
The protocol for implanting a TAVI requires a specific CT scan to evaluate the necessary size of the new valve, and to confirm that there is adequate access via the femoral route. The procedure is usually performed under sedation (no general anesthesia is required) and recovery is very fast.
In some cases (<10%) it is necessary to implant a pacemaker later if a heart rhythm disturbance is confirmed.
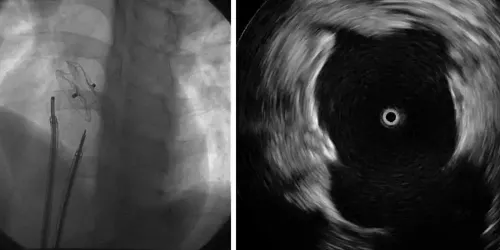
These interauricular septal defects can be repaired by catheterization in more than 95% of cases, when there is an indication for it. Specific devices made of a metallic alloy (nitinol), which are biocompatible and very effective, are usually used.
In the case of FOP, there is scientific evidence in favor of closing it in patients who have suffered a neurological problem (ictus) of unexplained cause. The effectiveness of the procedure and its safety are very high.
In the case of ASD, the defects are larger and require specific devices. The intervention is performed through femoral venous access and guided by transesophageal or intracardiac ultrasound, to confirm the correct positioning of the chosen device.
In both procedures the admission is usually only 24 hours and recovery is very fast.
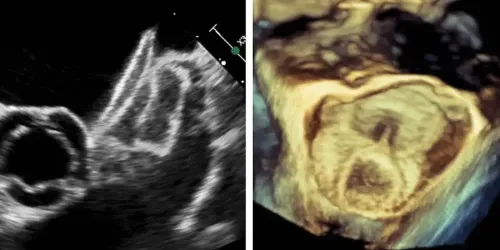
This technique is increasingly used to avoid taking anticoagulant drugs, especially in patients who have suffered severe bleeding due to anticoagulation (mainly digestive or cerebral bleeding).
It involves implanting a device that occludes the left ear, a small pocket inside the left atrium, where thrombi (clots) usually form, especially in patients who have arrhythmias such as atrial fibrillation.
The procedure is performed under general anesthesia and guided by transesophageal ultrasound, and is accessed through the femoral vein. The success rate is greater than 95%.
The discharge is usually early, after 24 hours, with a rapid recovery.
Do you need to request a consultation with one of our specialists?
INTERVENTIONAL CARDIOLOGY
Digitized Hemodynamics Room
The hemodynamics room is totally digitalized, it is called the catheterization or interventional cardiology laboratory, because more and more complex examinations and treatments are being carried out.

v
It evaluates the normal coronary artery wall, atherosclerotic changes in the anatomy and dimensions of the coronary artery.
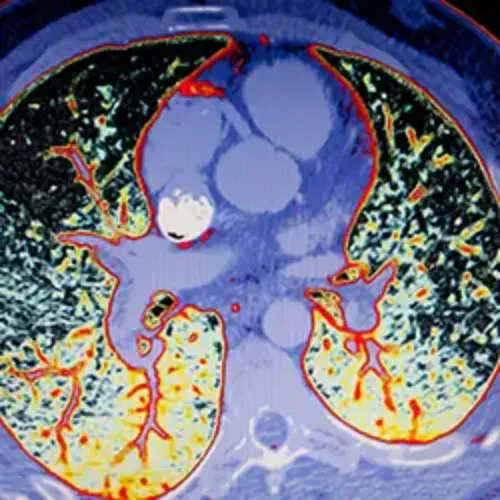
Virtual Histology
Color images that more clearly locate the fat (lipid) content of the atheroma plaque, better estimating its vulnerability.

Optical coherence tomography
A high-resolution image that uses light from a laser source to probe microscopic structures in biological tissues as a scanner.

Why at the Clinic?
- Cardiologists who are an international reference.
- State-of-the-art technology for maximum precision.
- Minimally invasive procedures for the prompt recovery of our patients.
Our team of professionals
Research
New advances in treatment
Research is a key part of the Department of Cardiology in its quest to offer the best patient care, which is why it has several clinical trials underway in relation to different cardiac pathologies.
Participating in these trials offers new possibilities to patients with access to the latest therapeutic advances.




