Osteoarthritis of the knee
"Osteoarthritis is often associated with overweight and/or the presence of angular deformities, especially in the knee. The moment for placing a prosthesis must be carefully considered".
DR. ANDRÉS VALENTÍ
DIRECTOR. ORTHOPEDIC SURGERY AND TRAUMATOLOGY DEPARTMENT

Osteoarthritis of the knee is a degenerative and "wasting" disease that occurs more often in older people, but can also occur in younger people due to previous knee injuries. The cartilage gradually wears away, reducing the protection of the bones.
The knee is one of the most common joints in the human skeleton to develop osteoarthritis.
The reason for the high frequency of osteoarthritis of the knee, compared to other joints in the body, is because the knee is a "load" joint, that is, it has to support the weight of the body and the objects we carry, when we stand or when we move around by walking, running, climbing or descending stairs.
Osteoarthritis of the knee generally develops slowly and the progression of the pain usually follows the same progression, although it can occur with spontaneous decompensations (primary osteoarthritis).
Sometimes the osteoarthritis is due to previous injuries of the knee as much ligamentosas as meniscales or of the cartilage, accelerating the appearance of the symptoms (secondary osteoarthritis).

What are the symptoms of osteoarthritis of the knee?
The fundamental symptom of the patient with knee arthrosis is pain. In the beginning, the pain is very mild, only appears when a very important physical activity has been carried out, and it quickly subsides with rest.
When the disease has become established, it is normal for the patient to notice greater discomfort when starting to walk, improving the symptoms after a while.
Added to the pain is a feeling of stiffness and difficulty in bending and extending the leg, which is also more intense after a long period of rest. Another symptom is the snapping sensation, which occurs when bending the knee.
The pain in the knee is greater when climbing and descending stairs, when the patient squats and when walking on uneven ground. In more severe arthrosis, the patient may notice symptoms even at rest.
With greater than usual physical effort (a longer walk, for example), the pain becomes more acute, continuous, and even the knee swells due to the formation of an effusion.
The most common symptoms are:
- Pain in the knee.
- Failure of the leg when carrying it.
- Inflammation of the joint.
- Stiffness of the joint.
In the cases in which more advanced phases of the disease are reached, besides the pain, that becomes more continuous and intense, the patient suffers a diminution in the movements that can make with the knee (for example, it cannot flex or extend the leg completely).
Certain deformities of the joint and alterations in the alignment of the bones may also appear, with arching of the lower limb. It is common for the patient to limp while walking and for the knee to weaken, with the patient frequently noticing a sensation of "failure" in the knee when taking steps.
Do you have any of these symptoms?
You may have osteoarthritis in your knee
What are the causes of osteoarthritis of the knee?
The age at which osteoarthritis usually begins to develop is around 50 years old and its progression is very slow.
The arthritis of knee is very rare in young people, unless they have suffered a previous problem in the articulation (fracture or traumatism, meniscal injury...) that favors the appearance of an arthritis like complication.
Obesity is another factor that has an important relationship with the development of osteoarthritis in the knees. It is easy to understand that in an obese person their knees have to support an overload of weight that favors a greater wearing down of the articulation.
In addition, osteoarthritis of the knee is more frequent in women than in men. The reason for this difference between the sexes is unknown.
Preventive measures
It is advisable:
- Move frequently, alternating with periods of rest.
- Frequent changes of position of the knees, making soft, constant, slow exercises of mobility of the same ones, insisting on the complete extension.
On long car/airplane trips, getting up every 2 hours to move your legs, especially stretching them well, etc.- Use low-heeled shoes with a firm buttress.
- Practice swimming and/or cycling without resistance.
- Use a firm mattress.
- Maintain the appropriate weight for your age and constitution.
- In inflammatory phase, application of local cold (never directly).
- Get in and out of the car with caution.
You will avoid:
- Going up and down stairs without necessity.
- Streets with a lot of slope.
- Being a long time with the knees bent.
- To walk in excess, especially by irregular land.
- Kneeling / squatting.
- Carrying weights.
- Turning and twisting with a fixed foot.
How is knee osteoarthritis diagnosed?
Diagnosing knee osteoarthritis is simple. It is based on the doctor's questioning of the patient about the characteristics of the symptoms, followed by an exploration of the knee joint, with the evaluation of its movements.
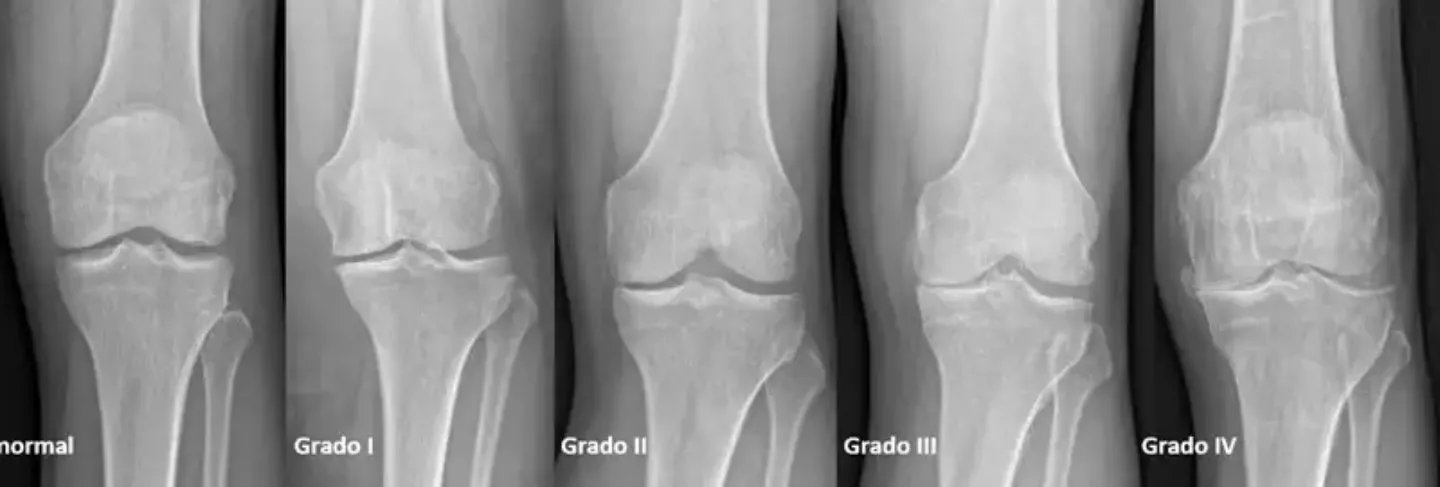
The diagnosis is confirmed through the practice of a knee x-ray, in which the doctor can see the unmistakable and characteristic signs of arthrosis, such as narrowing of the joint space, changes in the bone and the formation of bone spurs (osteophytes) .
Blood tests and so-called "rheumatic tests" are always normal in this disease.
Other tests, such as MRI or scans, may be needed to determine the condition of the bone and soft tissues or when a complication in the knee, or another knee injury not related to osteoarthritis (a torn meniscus, for example), is suspected.
Sometimes it is necessary to perform an arthroscopy to have a direct view of the problem.
How is a knee artrosis treated?
The aim of treatment is to relieve pain and maintain functional capacity
Medications
Painkillers, such as acetaminophen and anti-inflammatory drugs (NSAIDs) are often the first choice of treatment for osteoarthritis of the knee.
COX-2 inhibitors are a special type of NSAID that may cause fewer gastrointestinal side effects.
Corticosteroids are powerful anti-inflammatory agents that can be injected into the joint.
These injections provide temporary pain relief for decompensated situations and reduce inflammation; however, the effects do not last indefinitely.
Glucosamine, chondroitin sulfate, collagen... are substances that are naturally found in the joint cartilage and can be taken as supplements to relieve discomfort. There is no evidence to support that they are capable of reversing the progression of osteoarthritis.
Your doctor may recommend surgery if your osteoarthritis pain is disabling and not relieved by conservative treatments.
Arthroscopy: Two small incisions and specific instruments can be used to resolve meniscal and blockage problems that cause decompensation in the arthritic knee, although it is a procedure not often used to treat arthrosis of the knee.
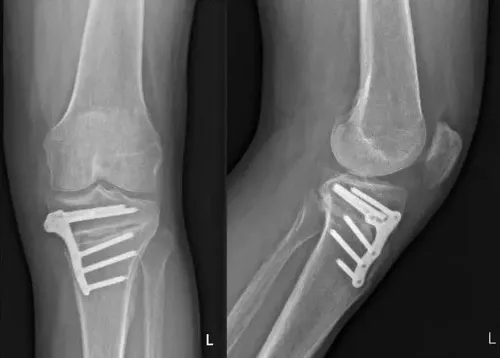
Osteotomy: Consists of making a controlled cut in the tibia or femur to correct or change the load axis and thus relieve pain, function and symptoms resulting from wear and tear on a part of the joint.
It is performed on knees with osteoarthritis or wear of a compartment and on young, active people.
Total or partial knee prosthesis (arthroplasty)
It consists of the partial or total replacement of worn joint surfaces to restore the function of the knee.
The Department of Orthopedic Surgery and Traumatology
of the Clínica Universidad de Navarra
The Department of Orthopedic Surgery and Traumatology covers the full spectrum of congenital or acquired conditions of the musculoskeletal system including trauma and its aftermath.
Since 1986, the Clinica Universidad de Navarra has had an excellent bank of osteotendinous tissue for bone grafting and offers the best therapeutic alternatives.
Organized in care units
- Hip and knee.
- Spine.
- Upper extremity.
- Pediatric orthopedics.
- Ankle and foot.
- Musculoskeletal tumors.

Why at the Clinica?
- Experts in arthroscopic surgery.
- Highly qualified professionals who perform pioneering techniques to solve traumatological injuries.
- One of the centers with the most experience in bone tumors.



















