Scoliosis
"With the new minimally invasive scoliosis correction techniques without fusion, spinal alignment is adjusted during the child's growth phase."
DR. EDUARDO HEVIA
SPECIALIST. ORTHOPEDIC SURGERY AND TRAUMATOLOGY DEPARTMENT

What is scoliosis?
Scoliosis consists of the lateral deviation or left or right deviation of the spine.
The spine is straight when viewed from the front or the back. When viewed in profile, the normal spine has four curves, two with posterior convexity, called normal kyphosis, and two with anterior convexity, called lordosis.
The cervical and lumbar areas have lordosis and the thoracic and sacral areas have kyphosis. Normally we speak of cervical lordosis, thoracic kyphosis and lumbar lordosis.
In more than 85% of the cases its cause is unknown. In the rest of the cases it is due to defects in the formation of the spine during the embryonic life or it is a sign that accompanies other general illnesses, such as muscular dystrophy or Marfan's Syndrome.

What are the symptoms of scoliosis?
Seen from behind a normal spine is straight, so that the back appears symmetrical.
When there is scoliosis, the spine is curved and one or more of these signs can be seen:
- One hip higher or bulging than the other.
- A shoulder blade (or "shoulder blade") higher or bulging than the other.
- One shoulder higher than the other.
- The head is not centered in relation to the hips.
- Standing, with arms hanging down, the space between one arm and the trunk is greater on one side than on the other.
- When bending forward with legs stretched out until the back is horizontal, one side is higher or bulging than the other.
The most common symptoms are:
- Muscle contractures.
- Deviation of the shoulders, back and hips.
- Back pain.
Do you have any of these symptoms?
You may have scoliosis
How is scoliosis diagnosed?
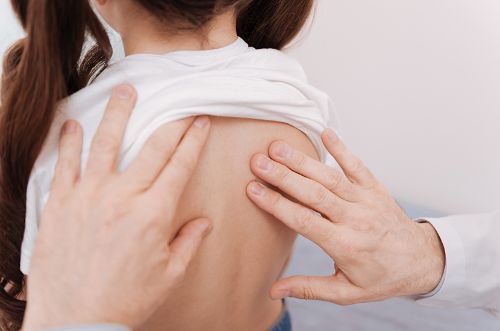
Scoliosis is usually suspected at a routine pediatric checkup.
When the pediatrician observes some of the symptoms to request a spinal x-ray to evaluate if there is spinal deviation and the degree of it.
Sometimes, the child or adolescent will be referred to the orthopedic surgeon for a more specific evaluation.
How is scoliosis treated?
Exercises and rehabilitation do not reduce the magnitude of the curve or the risk of progression, but these measures can be used as an adjunct treatment to improve posture and strengthen muscles.
Orthopedic treatment (brace/necklace) modifies the natural progression of adolescent idiopathic scoliosis and reduces the risk of progression. Orthopedic measures are the most effective treatment method with curves of less than 40° and one of the treatments of choice for growing age patients with curves of 20-40°.
Only a small number of patients with curves of less than 20º progress. Orthopedic measures do not prevent scoliosis progression in patients who have reached the end of the growth stage.
In 85-90% of cases, no surgical treatment is necessary.
Surgery may be necessary in case of very large curves with constant progression or if the patient requests a surgical intervention to improve his/her physical appearance (for aesthetic reasons).
Surgery can prevent progression and correct the deformity. Usually the surgeon uses metal implants (rods and screws/hooks/wires) to correct and hold the area of the deformity until the operated vertebrae have been joined (fused). Bone fusion ensures permanent stability.
Surgical treatment is usually indicated for growing patients with curves of more than 60° or 40-60° and evident progression despite treatment with orthopedic measures. If the patient considers that a curve of more than 40º is an unacceptable deformity, he or she can also be operated on.
Non-fusion techniques for treating scoliosis in children and adolescents
Innovative minimally invasive surgery that allows correcting spinal curves while preserving mobility. The rods are maintained during growth, taking advantage of the correction that occurs during it without fusing the bones of the spine. Upon reaching skeletal maturity (Risser 5), the rods are removed, leaving the spine corrected, without deformity, and with normal mobility.
- Targeted towards adolescent children (with growth potential) with curves between 35 to 60 degrees.
- By not permanently fixing the spine, it will maintain full mobility and allow for modulation of vertebral growth to prevent deformation.
- Additionally, the surgery is performed with computerized navigation, small muscle incisions, and minimally invasive techniques, enabling rapid recovery and preservation of muscle for mobility restoration.
IN NAVARRE AND MADRID



