Fractures of the proximal tibia
"Depending on the energy and mechanism, fractures can have very different degrees of complexity and prognosis".
DR. ANDRÉS VALENTÍ
DIRECTOR. ORTHOPEDIC SURGERY AND TRAUMATOLOGY DEPARTMENT

The proximal part of the tibia, belongs to the knee joint and its fracture occurs due to various traumas.
Young people often experience these fractures as a result of high-energy injury, falls from heights, sports injuries, and car accidents, although they sometimes occur due to excessive activity (stress fracture).
Older people may experience these types of fractures with low energy mechanisms due to poorer bone quality.
Sometimes, the fracture is accompanied by injuries in menisci and ligaments, aggravating the prognosis. The surgical treatment, when it is required, allows to restore the congruence of the articulation and to repair the associated injuries, diminishing the risk of generating an osteoarthritis.

What problems can occur after a fractured tibia?
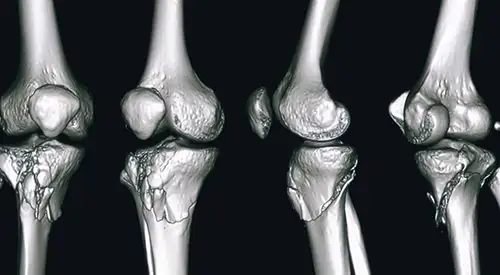
There are several types of proximal tibia fractures. The bone can be broken by a definite line or in many fragments (comminuted fracture).
The upper part of the tibia (the tibial plateau) is made of cancellous bone, which is less resistant. The impact often causes the bone to compress and remain sunken. This damage to the surface of the bone can cause misalignment of the limb, and over time can contribute to osteoarthritis, instability, and loss of knee motion.
Fractures of the proximal tibia can sometimes be open, which means that the skin is open with an increased risk of infectious complications.
The complications that can appear are:
- Incorrect alignment of the limb.
- Osteoarthritis.
- Instability.
- Loss of mobility of the knee.
Have you suffered a fracture of the proximal tibia?
Adequate treatment is important to prevent sequelae
How is a proximal tibia fracture diagnosed?
The most common way to evaluate a fracture is with X-rays, which provide clear images of the bone. X-rays can show the type of fracture and the treatment to be followed.
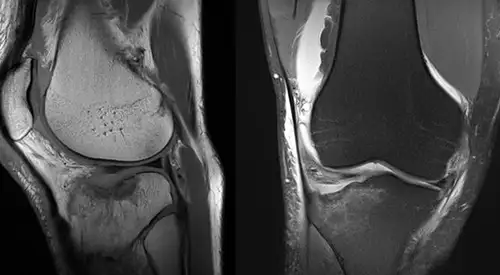
Sometimes, due to the complexity of the fracture, it may be necessary to perform a Computed Tomography (CT) scan that shows more details of the fracture or a Magnetic Resonance Imaging (MRI) to assess the existence of associated ligament or meniscal injuries.
How is a fractured tibia treated?
A fracture of the proximal tibia can be treated conservatively or surgically. There are benefits and risks associated with both forms of treatment.
The preferred treatment is based on the type of injury and the patient's needs, expectations, lifestyle and general conditions.
In an active individual, restoration of the joint through surgery is usually appropriate because it increases stability, mobility and minimizes the risk of osteoarthritis.
In other cases, where there is no displacement of the fracture or surgical treatment is a risk to the patient, conservative treatment by immobilization may be decided upon.
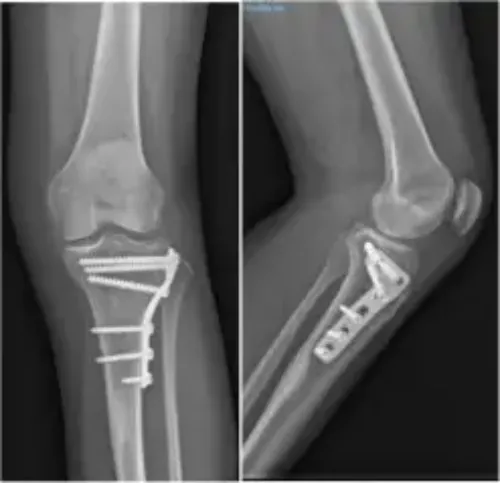
Surgical treatment for tibia fractures consists of reducing or replacing the fragments in place.
If the fracture affects the joint and sinks the bone, it may be necessary to lift the bone fragments to restore joint function.
When lifting these fragments, however, a space is created in the cancellous bone. This hole must be filled with material to prevent the upper bone from collapsing.
This material can be a bone graft from the patient or from a musculoskeletal tissue bank. Natural or synthetic products that stimulate bone healing can also be used.
Once the anatomy has been reconstructed, the fragments are synthesized and stabilized using plates and screws.
In some cases, the condition of the soft tissue due to inflammation or suffering is so bad that the use of plates could threaten it even more. The same happens in open fractures where there is a greater risk of infection.
The use of external fixators can be considered as a temporary or definitive treatment to solve the problem. The external fixator is removed when the injury is resolved.
Open fractures: If there is an open wound, the underlying fracture may be exposed to bacteria that could cause an infection.
Early surgical treatment will clean the fracture surfaces and soft tissues to decrease the risk of infection.
Compartment Syndrome: In a small number of injuries, the soft tissue swelling in the calf can be so severe that increased pressure threatens the blood supply to the muscles and nerves of the leg and foot. This is called compartment syndrome and may require emergency surgery.
During the procedure, called fasciotomy, vertical incisions are made to release the skin and muscle coverings.
These incisions are often left open and then stitched up days or weeks later as the soft tissues recover and the swelling goes down.
In some cases, a skin graft is required to help cover the incision and promote healing.
In the first days the control of pain and inflammation marks the good evolution of the fracture. Depending on the type of fracture and treatment performed, a more or less early mobilization of the joint will be decided (initially passive and later active).
The weight load on the extremity will also depend on the type of fracture and the degree of stability achieved with the treatment.
The beginning of the load and in a progressive way does not take place before the first six weeks and the complete load, around 3 months from the beginning of the treatment.
During this time, you will need crutches or a walker to move around. A rehabilitation plan will be designed to help you regain functionality as quickly as possible.
The Department of Orthopedic Surgery and Traumatology
of the Clínica Universidad de Navarra
The Department of Orthopedic Surgery and Traumatology covers the full spectrum of congenital or acquired conditions of the musculoskeletal system including trauma and its aftermath.
Since 1986, the Clinica Universidad de Navarra has had an excellent bank of osteotendinous tissue for bone grafting and offers the best therapeutic alternatives.
Organized in care units
- Hip and knee.
- Spine.
- Upper extremity.
- Pediatric orthopedics.
- Ankle and foot.
- Musculoskeletal tumors.

Why at the Clinica?
- Experts in arthroscopic surgery.
- Highly qualified professionals who perform pioneering techniques to solve traumatological injuries.
- One of the centers with the most experience in bone tumors.