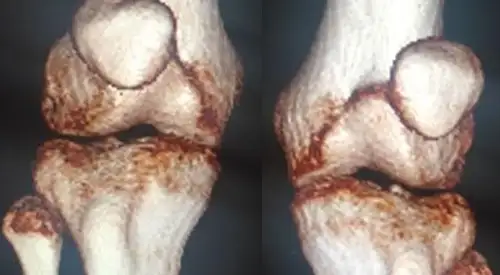
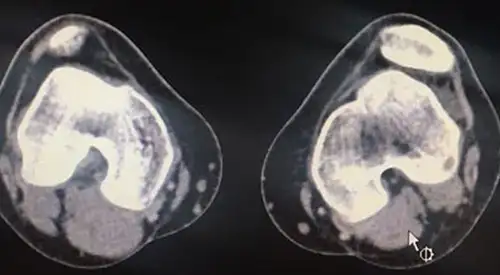
Instability or dislocation of the kneecap
"Once your knee has regained its movement and strength, your doctor will probably allow you to resume your activities normally. A full return to more demanding sports may take longer".
DR. ANDRÉS VALENTÍ
DIRECTOR. ORTHOPEDIC SURGERY AND TRAUMATOLOGY DEPARTMENT

When a first episode of dislocation of the kneecap occurs either partially or completely, it usually causes pain and loss of function.
Sometimes, the kneecap is reduced to its original position spontaneously without the need for maneuvers. In other cases, it remains dislocated laterally until reduction maneuvers occur.
In any case, after a first episode of dislocation will require treatment to relieve symptoms of inflammation and pain and make a temporary immobilization of the knee for proper healing of tissues.

What are the symptoms of kneecap dislocation?
The symptoms associated with a patellar dislocation depend on the intensity of the episode and its spontaneous reduction or not.
In general, this first episode, produces pain, inflammation, knee insecurity and if the kneecap remains dislocated, an evident aesthetic deformity of the knee due to the kneecap being located laterally.
The most common symptoms are:
- Pain.
- Inflammation.
- Instability of the knee.
Do you have any of these symptoms?
You may suffer instability or a dislocated patella
What are the causes of patellar dislocation?
There are several reasons why the kneecap may become unstable or dislocated. In many cases, the kneecap dislocates with a low-force mechanism due to an abnormality in the bone structure of the child's knee that is forming and growing.
A shallow trochlear femoral groove, valgus axes of the knee, or torsional changes in the lower limbs may make dislocation more likely.
Sometimes the soft tissues (muscles, ligaments ...) have more laxity or poor muscle tone, making it more prone to dislocation. This occurs more frequently in girls, and the problem can affect both knees.
Children with cerebral palsy and Down syndrome may have kneecaps that are frequently dislocated due to an imbalance and muscle weakness.
In other occasions, the patellar dislocations happen after a lateral traumatism or torsion in people without alterations in the commented structures . This incidence is more common in high-impact sports such as soccer.
How is kneecap dislocation diagnosed?
If the kneecap is put back in place, you should consult your doctor as soon as possible.
During the exam, your doctor will ask you about how the injury occurred and specific symptoms.
He or she will also evaluate the range of motion, axes, and imaging tests to confirm the diagnosis and possible origin.
X-Ray
This test detects skeletal abnormalities in the knee.
Magnetic Resonance Imaging (MRI) and Computerized Axial Tomography (CT)
These explorations are sometimes requested to assess the state of the cartilage, rotational bone alterations or if the presence of associated lesions is suspected as free bodies.
How is kneecap dislocation treated?
The immediate treatment is the reduction of the dislocation.
Initial phase: Immobilization and partial loading with crutches. Your doctor may recommend the use of an orthopedic brace for 3 to 4 weeks. This stabilizes the knee while injuries heal.
Recovery Phase: Application of physical therapies to decrease inflammation and begin muscle toning.
Subsequent rehabilitation attempts to achieve almost complete functional recovery, although there is a greater risk of new episodes in up to 40-60% of cases.
The kneecap often remains more unstable than before the injury. Recurrences are also common if the dislocation has non-correctable causes in a conservative manner.
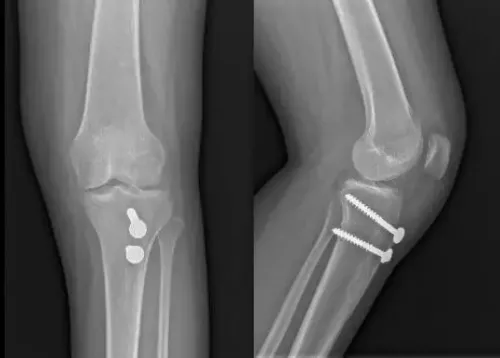
If the kneecap is dislocated several times, or remains unstable despite treatments, surgery may be recommended to correct the problem.
The surgical treatment allows to return to activities with full functionality and avoid in the future, the development of an early osteoarthritis of the kneecap and therefore a painful knee.
The type of surgery will depend on the cause that provokes the instability of the kneecap.
Surgical treatments often involve rebuilding the ligaments that hold the kneecap in place. This surgery is sometimes performed arthroscopically.
Repeated dislocation caused by congenital or other bone deformity may require more complex surgical treatment with changes in bone structure.
The Department of Orthopedic Surgery and Traumatology
of the Clínica Universidad de Navarra
The Department of Orthopedic Surgery and Traumatology covers the full spectrum of congenital or acquired conditions of the musculoskeletal system including trauma and its aftermath.
Since 1986, the Clinica Universidad de Navarra has had an excellent bank of osteotendinous tissue for bone grafting and offers the best therapeutic alternatives.
Organized in care units
- Hip and knee.
- Spine.
- Upper extremity.
- Pediatric orthopedics.
- Ankle and foot.
- Musculoskeletal tumors.

Why at the Clinica?
- Experts in arthroscopic surgery.
- Highly qualified professionals who perform pioneering techniques to solve traumatological injuries.
- One of the centers with the most experience in bone tumors.