Herniated thoracic disc
"The anterior approach to the spine has evolved a lot. Now, with minimal incisions and the use of endoscopy, we achieve very effective results with better patient recovery".
DR. VÍCTOR RODRIGO
DIRECTOR. NEUROSURGERY DEPARTMENT

What is a thoracic herniated disc?
The thoracic or dorsal disc herniation is a degenerative pathology of the spine. Although degenerative spinal pathology is a very common disorder throughout the population, the thoracic location of this type of problem is the most uncommon of the entire spine.
In addition, most disc herniations are under-diagnosed, and when they are diagnosed, treatment is usually conservative.
In the Clínica Universidad de Navarra we have implemented a new surgical technique for thoracic disc herniation. A minimally invasive surgery through endoscopy with which the postoperative time and recovery is much faster and less painful.

What are the symptoms of thoracic disc herniation?
The typical symptomatology of dorsal hernias is dorsalgia, which can be associated with pain in the hemicint or belt, as well as sensory and/or motor clinical pain in the lower limbs, including paraparesis and paraplegia. It can also cause sphincter dysfunction.
Other more uncommon symptoms are epigastralgia, nausea and chest pain.
Most common symptoms of thoracic disc herniation
- Back pain.
- Alterations in the strength and sensitivity of the extremities.
- Sphincter dysfunction.
Do you have any of these symptoms?
You may have a herniated dorsal disk
How is thoracic disc herniation diagnosed?
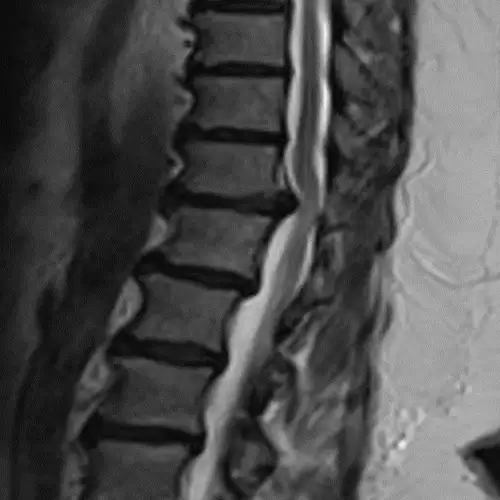
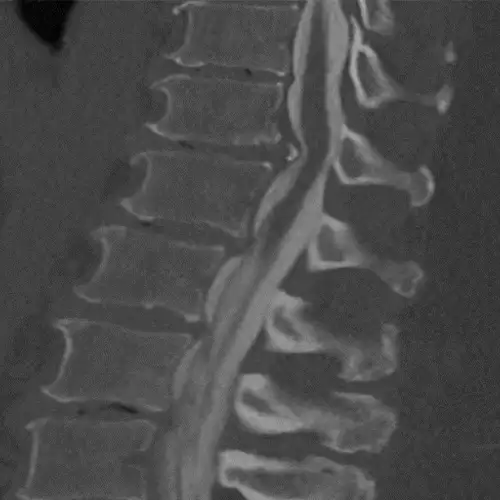
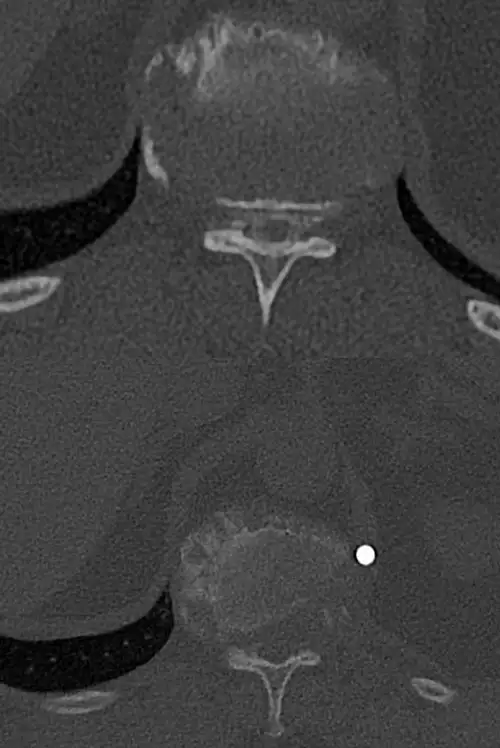
The diagnosis, in addition to being based on the symptoms and the physical examination by the specialist, is made like almost any spinal disease by means of magnetic resonance imaging (MRI), although it is usually complemented by computerized tomography (CT) and X-rays (Rx).
Sometimes contrast can be added to the intradural space in the CT and images of the spinal cord contour can be obtained (myelo-CT).
How is thoracic disc herniation treated?
Surgical treatment for thoracic disc herniation
The treatment is initially conservative with oral drugs, rehabilitative physical therapy and infiltrations and/or blockade; however, a percentage of these patients do not experience improvement, so surgery may be indicated.
Historically, the approach to the spine has been done later. These posterior thoracic approaches were not very effective at first, and in addition, they were associated with a high level of patient morbidity and mortality. With the passage of time, the antero-lateral approaches were corrected, which were truly more effective, but unfortunately the post-operative one was much more painful and arduous.
At present, the anterior approaches have been perfected, and smaller or minimal multiple incisions can be made through the use of microscopy and endoscopy. The main approaches we perform are:
- Transpleural endoscopic approach: Several small incisions are used in the antero-lateral thoracic area of the patient in lateral position and the lung cavity is accessed. By using an endoscope we can visualize the whole area to be treated and through the rest of the incisions we introduce the rest of the instruments to work.
- Exoscopic or microscopic retropleural approach: An incision of about 10 cm is used in the antero-lateral thoracic area of the patient in lateral decubitus and the previous area of the thoracic disc or vertebra to be treated is accessed.