Arthrosis
"The goals of treatment are to decrease the symptoms and disability of patients, improving the quality of life of those who suffer from the disease. The new treatments allow us to delay or even avoid the need for surgery".
DR. ENRIQUE ORNILLA
SPECIALIST. RHEUMATOLOGY SERVICE

What is osteoarthritis?
Osteoarthritis is the most common degenerative joint disease, characterized by the destruction of the hyaline cartilage that covers the bone surfaces.
The cartilage is a tissue that acts as a shock absorber by protecting the ends of the bones and promotes the movement of the joint. When osteoarthritis develops, this cartilage loses its properties. It can even disappear, causing the ends of both bones to rub directly, producing pain.
Usually it is located on the cervical and lumbar spine, certain joints of the shoulder and fingers, the joint of the root of the thumb, the hip, the knee, and the joint of the beginning of the big toe.

What are the symptoms of osteoarthritis?
The fundamental symptom is pain, which is insidious, deep and poorly located. This pain usually appears when an effort is demanded to the sick articulation and, in general, it worsens as the day advances. With the progress of the disease, the pain can appear with the rest or the nocturnal rest.
In the arthritis of the spine, it takes place pain of neck or the lumbar region, difficulty for the movement and contracture of the muscles of the affected region.
Another possibility, when the patient afflicts pain in the thigh (for irradiated pain), is that the arthritis is located in the hip.
Other symptoms are the articular deformities and the limitation of the mobility with pain to the pressure, clicks and crepitation of the articulation. The growth of the ends of the bones that form the joint can cause the joint to become larger and wider.
The most common symptoms are:
- Joint pain.
- Joint deformity.
- Inflammation in the joints.
- Stiffness.
Do you have any of these symptoms?
You may suffer from osteoarthritis
What are the causes of arthrosis?
It is not clear whether osteoarthritis is a single disease or a spectrum of pathologies with similar clinical and radiological manifestations.
Thus, we can classify osteoarthritis into two groups: primary, without a defined cause, and secondary, associated with other pathologies (hemochromatosis, gout, diabetes mellitus, bone dysplasia...).
Osteoarthritis related factors
Whether or not the ultimate cause of the disease is known, we can speak of a series of factors closely linked to its development:
- Systemic factors: sex, age, heredity, osteoporosis (hormonal state).
- Local factors: obesity, joint instability (laxity, deformities), repeated trauma, joint overload (occupational).
- Genetic factors: there is a series of genes closely associated with the development of osteoarthritis that can be studied by means of a simple saliva test.
How is osteoarthritis diagnosed?
There are no specific laboratory alterations of the osteoarthritis or any marker that allows a diagnosis or monitoring of the disease.
However, new markers of response to treatment are being investigated and are likely to be used in the coming years. There is also a genetic test that analyzes the main genes associated with advanced knee osteoarthritis and allows for earlier treatment.
To the physical exploration, deformities can be observed articulations, by increase of the osseous and capsular component and limitation of the mobility with pain to the pressure, clicks and crepitation of the articulation.
The growth of the ends of the bones that form the joint can cause the joint to enlarge and widen.
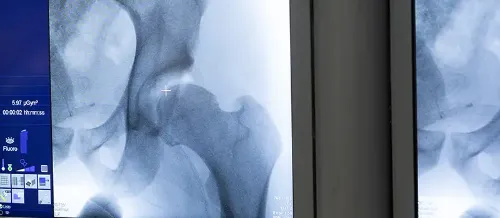
Radiology in the early stages may be normal, although typically there is a narrowing of joint space associated with subchondral sclerosis, appearance of marginal osteophytes (bony prominences), cysts, and abnormalities of bone contour.
How is osteoarthritis treated?
The goal of treatment is to relieve pain and maintain functional capacity
The therapies currently available are:
Non-pharmacological treatment: physical therapy, aerobic exercise (swimming, walking).
- Pharmacological treatment: as a first option, paracetamol
- As non-steroidal anti-inflammatory drugs, COX-2 inhibitors (celecoxib and rofecoxib) tend to be used. At times may be other analgesics such as tramadol or codeine.
- Glucosamine sulfate and chondroitin sulfate stimulate extracellular matrix synthesis of cartilage and appear to exert moderate control over joint pain, although studies have not shown completely conclusive results. Intra-articular steroids may be effective in specific cases.
- Hyaluronic acid and intra-articular platelet growth factors serve to treat those patients with osteoarthritis refractory to medical treatment by having an analgesic-anti-inflammatory and tissue-protecting effect.
Indicated in the late stages of the disease when there is refractory pain or significant functional disorder.
There are four surgical procedures: osteotomy (to correct the distribution of loads); arthroscopy (with intra-articular washing and debridement); arthrodesis (or joint fusion, useful in spine and small joints); and arthroplasty or joint replacement by a prosthesis, very often hip prosthesis and knee prosthesis.
The Rheumatology Service
of the Clínica Universidad de Navarra
The Rheumatology Service has a multidisciplinary team highly specialized in the diagnosis and treatment of rheumatological diseases, from osteoarthritis, arthritis or osteoporosis to autoimmune or inflammatory diseases.
In addition, we have doctors specialized in assisting pregnant women with autoimmune diseases, in order to guarantee the maximum safety of the fetus.
Organized in specialized units
- Inflammatory arthropathies.
- Degenerative arthropathies.
- Microcrystalline arthropathies.
- Bone pathology.
- Systemic autoimmune diseases.
- Autoinflammatory diseases.

Why at the Clinica?
- Valoración integral del paciente.
- Diagnóstico personalizado.
- Tecnología de vanguardia.



