Pneumothorax
"Currently, the most widely used surgical technique is videothoracoscopy with resection of subpleural apical bullae and pleural abrasion with gauze".
DR. ALEJANDRA DE LA FUENTE
SPECIALIST. THORACIC SURGERY DEPARTMENT

What is a pneumothorax?
Pneumothorax occurs when air leaks into the space between the lungs and the chest wall.
The pleural cavity is the space between the lung and the rib cage.
This air pushes on the outside of the lung and causes it to collapse. In most cases, only a portion of the lung collapses.
Tension pneumothorax is an emergency that requires immediate treatment.

What are the symptoms of pneumothorax?
It depends on the patient's functional reserve, so that in 5-10% of cases they are asymptomatic.
Chest pain (sudden onset, acute and unilateral) and dyspnea (difficulty breathing) are the most frequent symptoms (80-90% of cases). Dyspnea can be very intense in those patients with a very compromised functional reserve due to a basic pulmonary pathology. Other symptoms that may appear are dry cough, hemoptysis (coughing up blood), syncope and the perception of a noise in the chest when breathing.
In 3% of cases, what is called a tension pneumothorax occurs when the pressure in the pleural space exceeds the atmospheric pressure. This occurs when there is a valve mechanism that allows air to enter the pleural cavity during inspiration, without emptying during expiration. This causes a total collapse of the lung on that side, with a mediastinal shift that prevents venous return with consequent heart failure.
This condition is a vital emergency characterized by severe dyspnea, tachypnea (increased breathing rate), cyanosis, sweating, hypotension and bilateral jugular distension, requiring immediate decompression.
The most common symptoms are:
- Chest pain.
- Dyspnea.
- Dry cough.
- Hemoptysis.
- Syncope.
Do you have any of these symptoms?
You may have a pneumothorax
What are the causes of pneumothorax?
There are different types of pneumothorax depending on the cause that produces them:
- Iatrogenic pneumothorax, when it occurs after diagnostic or therapeutic instrumental manipulation.
- Traumatic Pneumothorax, in cases of previous thoracic trauma.
- Pneumothorax in relation to mechanical ventilation or barotrauma.
- Spontaneous pneumothorax, in which there is no apparent cause. Within this we find the primary or juvenile pneumothorax, which is usually related to the rupture of apical bullae; these consist of small lung cysts of unknown cause, although they usually occur in tall individuals with elongated chest.
We also call secondary pneumothoraces to those that appear in patients with basic pulmonary pathology such as COPD, exacerbations of asthma, pulmonary fibrosis of various causes, connective tissue diseases, endometriosis, necrotizing pneumonias, tuberculosis and in pneumonia in patients with AIDS.
How is pneumothorax diagnosed?
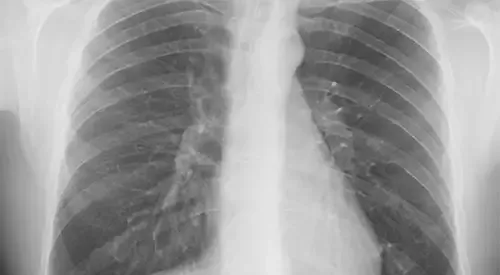
The diagnosis of pneumothorax is made by the symptoms, in addition to the physical and radiological examination.
In the physical examination it can be appreciated tachypnea, decrease or abolition of the physiological vesicular murmur to the auscultation, as well as tympanism to the percussion of the thorax and decrease of the vocal vibrations.
The diagnosis is confirmed with the performance of a chest X-ray (preferably performed in forced expiration), in which the lung collapse is appreciated.
How is pneumothorax treated?
Correct treatment should be aimed at preventing recurrences or reappearances of the pneumothorax.
It is carried out with different techniques, among which are chemical pleurodesis through the drainage tube (consisting of the introduction of talc or tetracyclines into the interpleural space in order to produce adhesions between the visceral and parietal pleura) and surgery.
Surgical indications are reserved for recurrent spontaneous pneumothoraces (after a second episode), persistent air leakage (more than 5-7 days), bilateral pneumothoraces and after a first episode in people with a higher risk of recurrence (pilots, divers,...).
The most widely used surgical technique is video-phthoracoscopy with resection of subpleural apical bullae and pleural abrasion with gauze (or alternatively):
- Scarification with electrocoagulation, laser or argon.
- Chemical pleurodesis with sterile talcum powder or by means of tetracyclines).
Relapses after videothoracoscopic surgery are around 5%. In the exceptional cases where the technique described above fails, the treatment of choice is the removal of the parietal pleura or pleurectomy through an axillary thoracotomy (with recurrence figures of less than 1%).
The Thoracic Surgery Service
of the Clínica Universidad de Navarra
The Thoracic Surgery Service of the Clinica Universidad de Navarra is composed of a team of medical specialists, nurses and health professionals specialized in the management of thoracic pathology.
In most procedures we perform minimally invasive surgery or videothoracoscopy for the diagnosis and treatment of numerous pleural, pulmonary and mediastinal lesions.
We maintain a close collaboration with other departments of the Clinic, among which Medical Oncology, Pneumology, Pathological Anatomy, Internal Medicine and ICU stand out.
Treatments we perform
- Lung cancer surgery
- Hyperhidrosis and facial flushing surgery
- Pleural surgery
- Mediastinal surgery
- Lung emphysema surgery
- Pleural mesothelioma surgery
- Lung metastasis surgery

Why at the Clinica?
- Medical specialists who are national references.
- Specialized nursing team.
- We work together with Pneumology and Medical Oncology.

